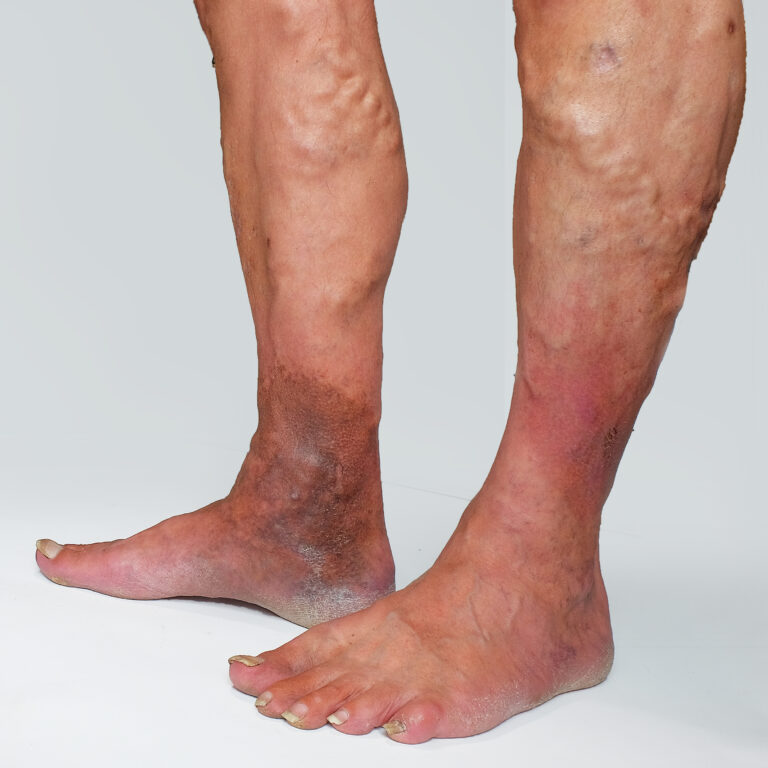
Lipodermatosclerosis
We provide structured assessment and treatment planning designed to stabilise disease progression, improve symptoms, and prevent complications.
Lipodermatosclerosis is a progressive inflammatory skin condition caused by long-standing venous hypertension. It can lead to pain, skin hardening, pigmentation changes, and increased risk of venous ulceration if not managed early.
What is lipodermatosclerosis?
Lipodermatosclerosis develops when sustained venous pressure causes inflammation and fibrosis in the lower leg tissues. Over time, this leads to:
- skin tightening and induration
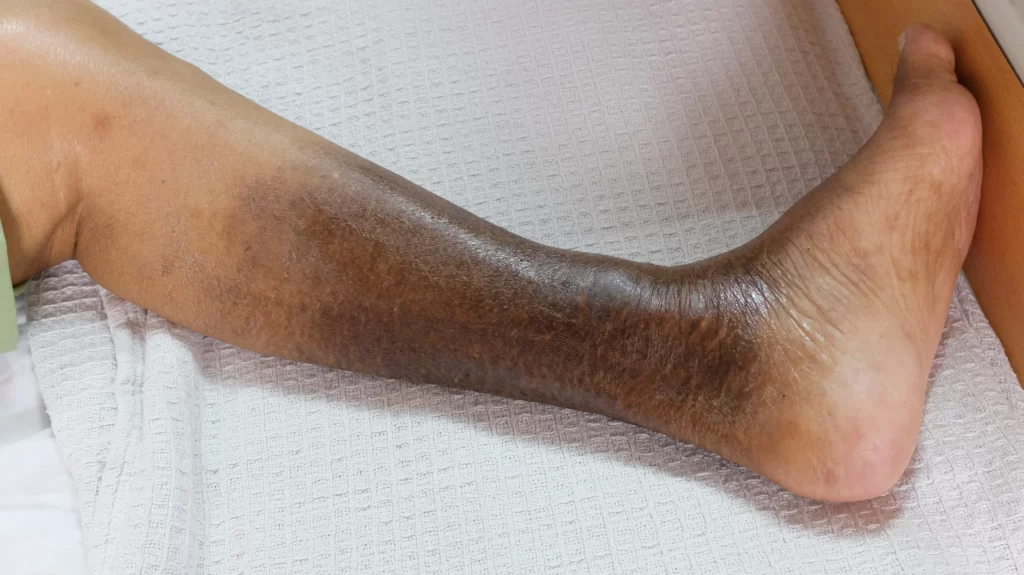
- brown or red pigmentation changes
- tenderness in the lower leg
- ankle narrowing (“inverted champagne bottle” appearance)
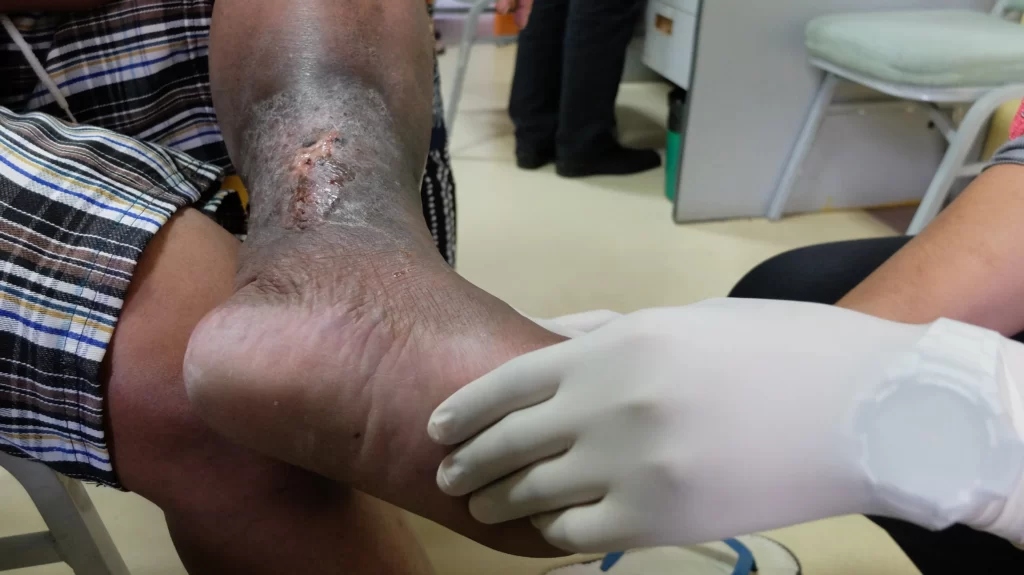
- increased risk of venous ulceration
Early intervention can slow progression and reduce long-term skin damage.
Who should attend this clinic?
You may benefit from assessment if you have:
- tightening or hardening of the lower leg skin
- persistent ankle inflammation or tenderness
- brown or reddish pigmentation around the gaiter region
- recurrent cellulitis in the lower leg
- venous eczema or skin thickening
- previous or threatened venous ulceration
These features often indicate advanced venous hypertension requiring targeted management.
Our role as your diagnostic gateway
Our clinic provides a structured pathway rarely available in standard vein services. We support patients at a critical stage where timely intervention can prevent permanent skin damage and chronic ulcer formation.
Following evaluation:
- A personalised management plan is created
- Compression therapy is optimised
- Underlying reflux patterns are documented and explained
- Ulcer prevention strategies are initiated if required
- Referral for advanced venous intervention is arranged where appropriate
This structured pathway helps stabilise disease and reduce long-term complications.