Heavy legs
swollen ankles
Deeper Understanding.
PREMIUM ASSESSMENT FOR LEG SWELLING & VEIN HEALTH
Swelling in the legs and ankles is often more than cosmetic. We look beyond the surface to identify whether swelling may be linked to venous pressure, reflux or other vein-related patterns.
EXPERT CLINICAL CARE | ADVANCED IMAGING | PERSONALISED TREATMENT
Common signs that swelling may be connected to your veins
Swollen ankles by the end of the day
Heavy tight uncomfortable legs
Skin marks, indentation or pressure lines
Swelling with visible veins or recurrence
We help you understand whether swelling is temporary — or a sign of something more
Presistent or recurrent swelling can be linked to venous pressure, reflux or chronic venous dysfunction. Our thorough assessment identifies the cause so we can treat what matters and protect your long-term leg health.
VENOUS PRESSURE
Vein volves may not be working efficiently. causing fluid to pool.
REFLUX & BACKFLOW
Blood flows the wrong way, increasing pressure in leg veins.
FLUID BUILD-UP
Fluid escapes into surrounding tissues, causing swelling
SKIN & TISSUE IMPACT
Ongoing pressure can offect skin, comfort and circulation.
Laurel clinical Approach
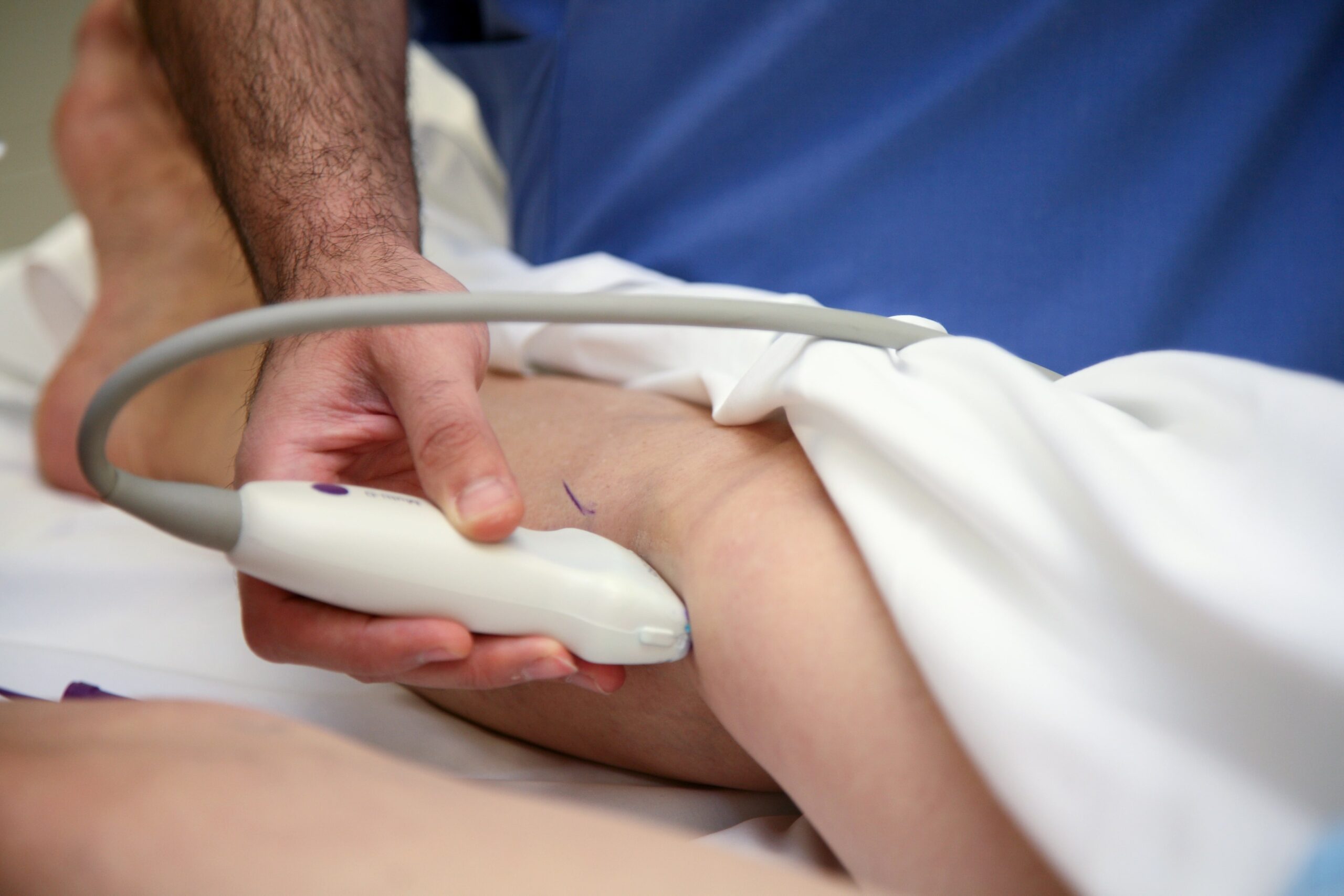
Our Pressure & Swelling Assessment
Understand the pattern
We listen carefully and roview your symptoms, history & litestyle.
Map the pressure source
Duplex ultrasound pinpoints reflux, blockages or other pressure drivers
Treat what matters
Torgeted, minimally invosive treatments address the foot cause, not just symptoms.
Protect long-term leg health
Care plans designed to reduce recurrence and support lifelong vascular health

Ready to understand what is really driving your vein symptoms?
Book a comprehensive assessment for heavy legs, swelling, skin changes, or recurrent veins.