skin changes in Venous disease
At Laurel Clinical, we understand the journey of living with chronic venous insufficiency (CVI) and the toll it can take on daily life. It often leads to changes in the skin such as discoloration, thickening, and even ulcers. Our team is here to help by addressing both the underlying causes and the symptoms associated with CVI.
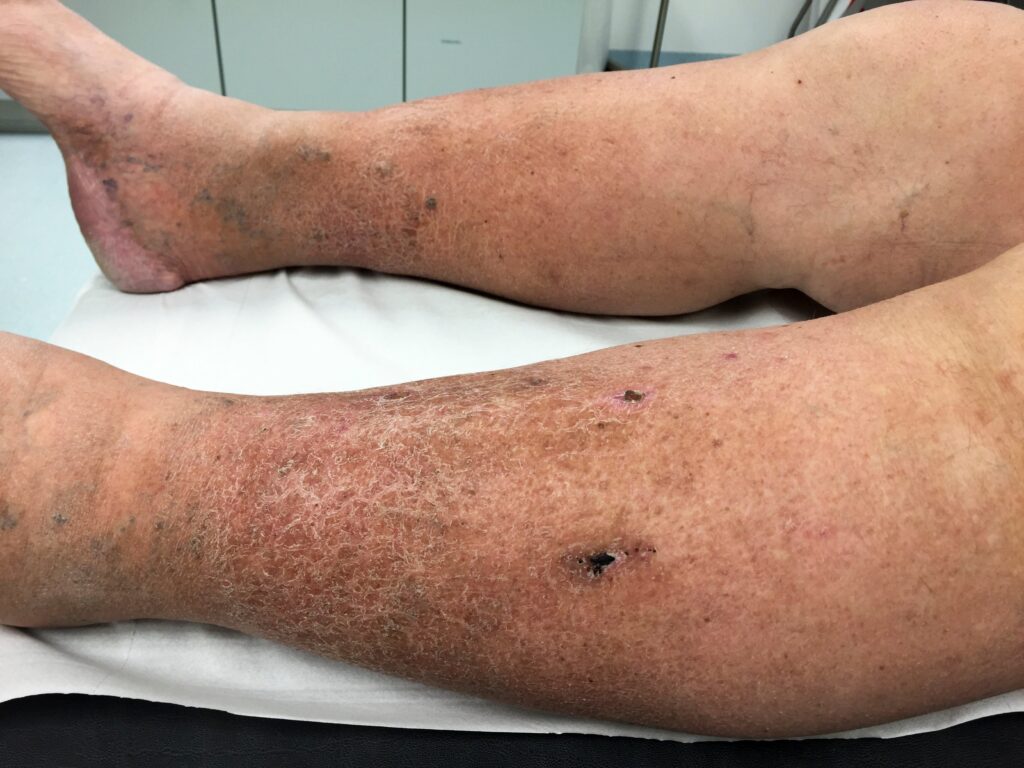
What Cause Skin Changes in Venous Disease?
In a healthy body, the veins in our legs work hard to carry blood back up to the heart, helped along by tiny valves that keep everything flowing smoothly in the right direction.
When these valves weaken or stop working as well, allowing blood to start pooling in the veins. This extra pressure on the vein walls and nearby tissues forces fluid to leak into the skin, causing inflammation, skin damage, and making it harder for wounds to heal properly.
A Personalized Approach from the start
Our approach goes beyond symptom management to address the underlying causes and provide comprehensive, tailored care that supports long-term healing and well-being.
In our personalized approach to venous disease treatment, we begin with a thorough assessment to understand the specific symptoms and health factors each patient is experiencing.
Using advanced diagnostics, we can identify the underlying issues contributing to skin changes, such as vein dysfunction or chronic inflammation
We work closely with each patient to guide them on daily practices that promote healing, from proper skin care routines to tips for enhancing circulation through activity and leg elevation.
Our team remains available for ongoing support, providing follow-up care and guidance to ensure that our patients can maintain the results of their treatment and prevent future skin complications.
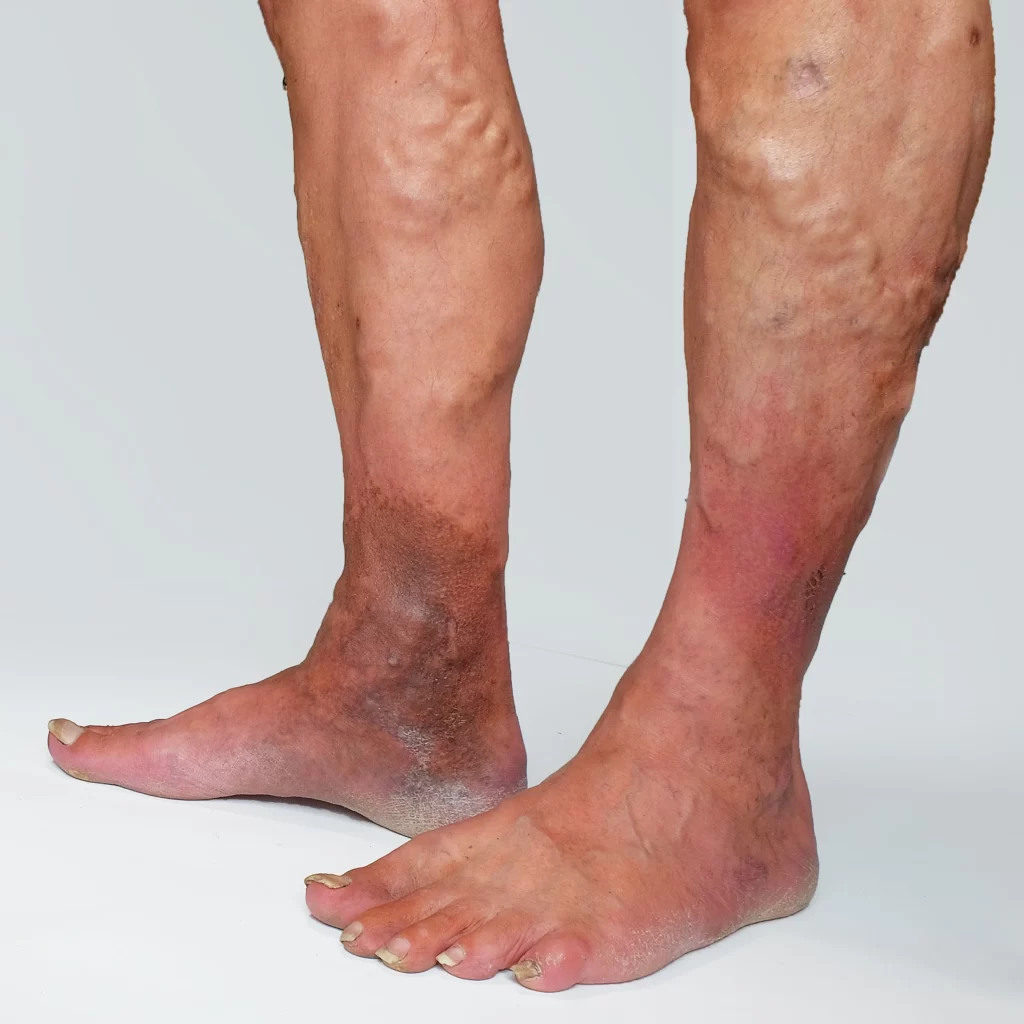
common skin changes
Discoloration
Thickened and Hardened Skin (Lipodermatosclerosis)
Venous Ulcers
Itching and Flaking
core components of our treatment
Key features of our combination approach includes:
Minimally Invasive Intervention
Procedures like sclerotherapy and endovenous laser ablation (EVLA) close off damaged veins, allowing blood to flow through healthier ones and relieving the pressure that causes discoloration, thickening, and even ulcers.
Surgical intervention
For patients with ulcers that don’t respond to less invasive treatments, surgical intervention can be a valuable step toward healing.
topical treatment
Topical treatments play an important role in managing skin changes caused by venous disease, offering relief from symptoms like dryness, itching, and inflammation.
medical Laser technology
Laser technology offers an effective solution for addressing skin changes and staining caused by venous disease. By targeting the pigments in discolored skin and damaged blood vessels, lasers help reduce visible redness, brown staining, and other pigmentation irregularities that often accompany venous issues.
Compression Therapy
Compression therapy is an essential part of treating skin diseases related to vein disease, as it improves blood flow and reduces venous pressure. This not only alleviates symptoms like swelling and discomfort but also supports the skin’s healing process by delivering nutrients more effectively