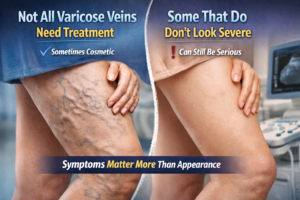
Varicose veins are swollen, twisted, enlarged veins that often make their presence known on our legs, They are not just a cosmetic concern for many. They sometimes appear with spider veins and dismissed as cosmetic concerns. Beyond their unsightly appearance, varicose veins can be a source of significant discomfort and pain, affecting daily activities and quality of life. But what exactly causes this pain, and how can it be managed, treated or how can you stop varicose veins? Let’s delve into the details.
The Painful Reality of Varicose Veins and Enlarged Veins
Varicose veins occur when your veins become enlarged, dilated, and overfilled with blood. Primarily affecting the legs and feet. Clinically, varicose veins are swollen and raised, with a bluish-purple or red colour and often accompanied by spider veins. The condition is often a result of faulty valves within the veins, leading to poor blood flow back to the heart.
Symptoms and Discomfort
Many individuals with varicose veins may experience a range of symptoms, including:
– Aching leg pain: A constant dull ache is common with severe varicose veins, especially after prolonged standing or sitting, which exacerbates the pressure within the varicose veins.
– Heaviness and fatigue: Legs can feel unusually heavy and tired with varicose veins, a sensation that worsens as the day progresses.
– Itching: The skin around varicose veins can become itchy, signalling potential skin changes or inflammation.
– Swelling: Fluid accumulation in the lower legs, especially around the ankles, is common with varicose veins, contributing to a sense of discomfort.
– Cramping and throbbing: Some people report experiencing muscle cramps and a throbbing sensation in the legs.
– Restless legs: Varicose veins can be linked to restless leg syndrome, a condition that causes an irresistible urge to move the legs.
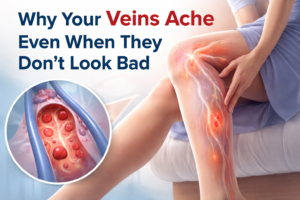
Understanding the Pain
The pain from varicose veins is primarily due to the increased pressure within vein walls of the affected veins. As the blood pools in these veins, it leads to inflammation and stretching of the vein wall, which can irritate nearby nerves. In more severe cases, varicose veins can lead to more serious complications, such as skin ulcers or blood clots, which can further exacerbate pain and discomfort. This is one of the most common reason to treat varicose veins.
Pain in the blood vessels, often referred to as vascular pain, can be felt due to various reasons and conditions affecting the vascular system itself—the network of blood vessels in the body, including arteries, veins, and capillaries. Understanding how people can feel pain in their vessels involves a look at the different mechanisms and conditions that can lead to vascular pain.
Mechanisms of Vascular Pain
1. Inflammation: Inflammation is a common cause of vascular pain in varicose veins. Conditions like vasculitis (inflammation of the blood vessels) can cause the walls of the vessels to swell, leading to pain. Inflammatory processes can irritate the nerve fibers surrounding the vessels or within their walls, transmitting pain signals to the brain.
2. Reduced Blood Flow: Conditions that reduce or block blood flow can cause pain. For instance, peripheral arterial disease (PAD) occurs when arteries become narrowed or blocked by fatty deposits, reducing blood flow to the limbs. This can cause muscle pain or cramping, particularly during physical activities, because muscles aren’t receiving enough oxygen.
3. Expansion or Stretching: An aneurysm, which is an abnormal bulge in the wall of an artery, can cause pain if it stretches the vessel wall. The stretching of the vessel can activate pain receptors (nociceptors) in the arterial wall, signaling pain.
4. Blood Clots: Thrombosis (the formation of a blood clot within a blood vessel) can cause pain by obstructing blood flow, leading to tissue damage and inflammation in the affected area. Deep vein thrombosis (DVT), for example, often causes pain and swelling of deeper veins in the legs.
Understanding Vascular Pain
– Receptors and Nerves: Blood vessels contain pain receptors (nociceptors) that can respond to various stimuli, including chemical, mechanical, and thermal changes. When these receptors are activated, they send pain signals through peripheral nerves to the central nervous system, where the brain interprets them as pain.
– Neurotransmitters and Inflammatory Mediators: During inflammation or injury, various substances such as prostaglandins, bradykinin, and cytokines are released. These substances can stimulate nociceptors or make them more sensitive to stimuli, amplifying the sensation of pain.
Conditions Associated with Vascular Pain
– Vasculitis: Involves inflammation of the blood vessels and can cause pain, along with other symptoms depending on the vessels involved.
– Peripheral Arterial Disease (PAD): Causes pain in the legs during exercise due to reduced blood flow.
– Aortic Dissection: A serious condition where the inner layer of the aorta tears, causing intense and sudden pain in the chest or back.
– Deep Vein Thrombosis (DVT): Formation of a clot in a deep vein, typically in the leg, causing pain and swelling of affected vein.
– Raynaud’s Phenomenon: Causes episodes of reduced blood flow to the fingers and toes, leading to pain and colour changes.
Varicose eczema associated with Varicose Veins
The skin disease known as varicose eczema, which is often referred to as venous eczema or stasis dermatitis, is a disorder that typically affects the lower legs and is frequently linked with varicose veins. Inadequate circulation and accumulation of blood in the veins are the causes of this condition, which ultimately results in elevated pressure and fluid loss. Those who do not seek treatment may experience the skin becoming red, itchy, bloated, and discoloured. Additionally, the skin may become dry, flaky, or develop weeping sores.
It is possible for the pain that is connected with varicose eczema to originate from the varicose veins that are under the skin. This may result in hurting, discomfort, and a heavy feeling in the legs, especially after standing for extended periods of time. This may have a substantial influence on the quality of life of an individual.
When treating varicose eczema, it is necessary to treat not just the skin disease but also the venous problems that are underlying the condition. Compression therapy, skin care, medicine, treatment for varicose veins, elevating the legs, exercise, and avoiding standing for lengthy periods of time without moving are some of the methods that may be used to manage this disease.
Managing and Treating Varicose Vein Pain
Fortunately, there are several strategies and treatments available for managing the discomfort discomfort and relieverelieve symptoms associated with varicose veins:
Lifestyle Changes and Home Remedies
– Exercise regularly to improve blood circulation in the legs. Walking is particularly beneficial.
– Elevate your legs whenever possible to relieve symptoms and reduce pressure in the varicose veins.
– Avoid prolonged standing or sitting to prevent blood from pooling in the developing varicose veins.
– Wear compression stockings to improve blood flow and reduce pain and swelling from the varicose veins.
Medical Treatments for Treating Varicose Veins
– Sclerotherapy: A solution is injected into the varicose veins, causing it to scar and helps blood flow to reroute through healthier veins.
– Endovenous laser therapy (EVLT) or radiofrequency ablation: These minimally invasive procedures use heat to close off the affected varicose veins.
– Vein stripping: A surgical procedure to remove varicose veins, typically reserved for severe cases.
What’s the worst that can happen with varicose veins?
While varicose veins are often considered a cosmetic issue, they can lead to more serious health complications if left untreated. Some of the potential severe outcomes associated with varicose veins are:
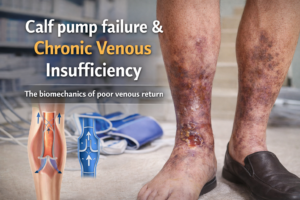
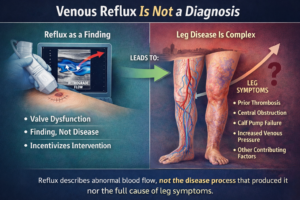
1. Chronic Venous Insufficiency (CVI): Over time, you develop varicose veins which can lead to chronic venous insufficiency, where your veins struggle to send blood from your legs back to your heart. This can cause swelling, pain, and changes in skin color.
2. Ulcers: Venous ulcers can develop on the skin near varicose veins, particularly around the ankles. These ulcers are painful and can be difficult to heal. They occur due to long-term fluid build-up in the tissues, which breaks down the skin, leading to an ulcer.
3. Superficial Thrombophlebitis: Varicose veins can cause superficial thrombophlebitis, which is inflammation of a vein just under the skin, typically resulting from a blood clot. This condition can cause pain, redness, and swelling.
4. Deep Vein Thrombosis (DVT): Although less common, people with varicose veins can develop complications from DVT, which is a blood clot in a deeper vein. This condition can be life-threatening if the clot breaks loose and travels to the lungs, causing a pulmonary embolism.
5. Bleeding: The skin over varicose veins is often thin and can bleed heavily if injured. Even a minor scratch or bump can lead to significant blood loss.
6. Lipodermatosclerosis: This condition involves the hardening of the fat and skin just above the ankle, leading to changes in skin color, pain, and the skin becoming tender to the touch.
The Importance of Seeking Medical Advice
If you’re experiencing pain or any other symptoms associated with varicose veins, it’s crucial to consult with a healthcare professional. They can provide a thorough evaluation to prevent varicose veins and recommend the best course of action based on your specific condition. Ignoring symptoms can lead to worsening of the condition and increased risk of complications.
Conclusion
While varicose veins can indeed cause pain and discomfort, understanding the condition and taking appropriate action can significantly alleviate symptoms and improve quality of life. Whether through lifestyle modifications, home remedies, or medical interventions, it’s possible to manage the discomfort associated with varicose veins and lead an active, pain-free life.