No More Suffering in Silence: Discovering the Causes of Varicose Vein Pain
Are you tired of suffering in silence with the pain of varicose veins? You’re not alone. Many people face the discomfort and frustration that comes with this common condition. But what exactly causes varicose vein pain? In this article, we will explore the underlying reasons behind this discomfort and discuss effective ways to find relief.
Varicose veins are enlarged and twisted veins that most commonly occur in the legs and feet. They often appear as blue or purple bulging cords under the skin. While they are primarily a cosmetic concern for some, others experience pain, swelling, and aching in the affected area.
The causes of varicose vein pain can vary. One common factor is faulty valves within the veins, which disrupt the flow of blood and lead to congestion and pressure. This can result in the development of varicose veins and the associated pain. Other potential causes include obesity, pregnancy, genetics, and prolonged periods of standing or sitting.
Understanding the causes of varicose vein pain is the first step towards finding effective treatment options. By addressing the underlying issues, you can alleviate discomfort and improve your quality of life. Let’s dive deeper into this topic and discover effective solutions for treating varicose veins and minimising pain.
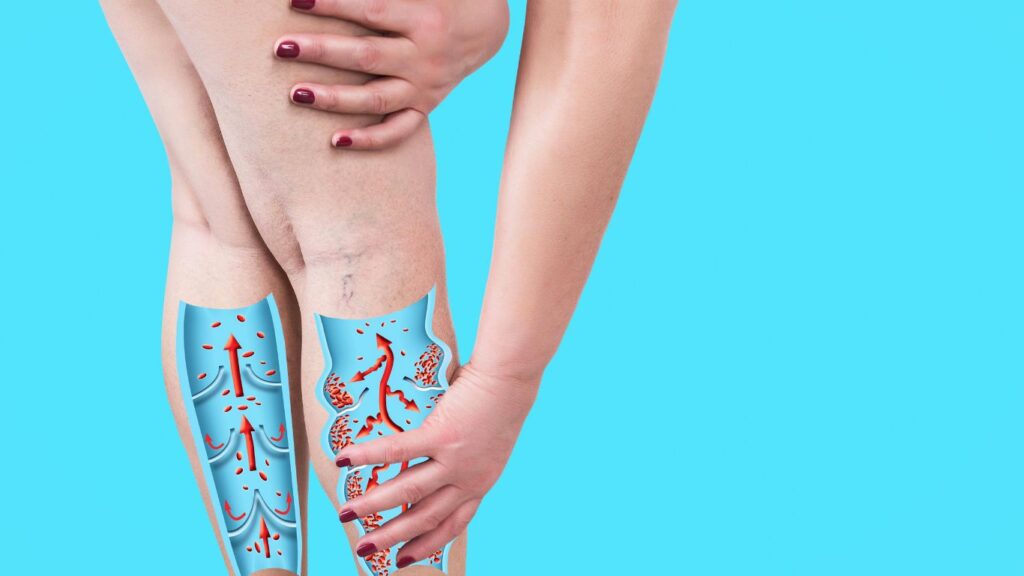
Why Do Varicose Veins Hurt?
Understanding the causes of varicose vein pain
Varicose veins are enlarged, twisted veins that commonly occur in the legs. When these veins become varicose, they often lead to localized inflammation, which can be a source of discomfort and pain.
The inflammation in varicose veins is primarily caused by the impaired flow of blood. Normally, blood is efficiently pumped back to the heart through a network of veins. However, in varicose veins, the valves that help regulate blood flow become weakened or damaged. This results in blood pooling or stagnating in the affected veins.
As blood accumulates in these veins, it exerts increased pressure on the vein walls. This heightened pressure triggers a series of responses from the body, including the release of inflammatory mediators. These mediators are chemical substances that promote inflammation, causing the affected area to become red, swollen, and tender.
Additionally, the stagnant blood within the varicose veins can lead to the leakage of fluid and blood cells into the surrounding tissue. This further contributes to the localized inflammation and discomfort.
The combination of increased pressure, inflammatory responses, and fluid leakage results in pain around the varicose veins. This pain may be described as aching, throbbing, or a feeling of heaviness. It can range from mild discomfort to more severe, debilitating pain, particularly after prolonged periods of standing or sitting.
Managing the pain associated with varicose veins due to localized inflammation often involves a combination of lifestyle modifications, compression therapy, and, in some cases, medical interventions. Seeking advice from a healthcare professional is crucial to determine the most appropriate treatment plan based on the severity of the condition.
Risk factors for developing varicose veins
In addition to the causes mentioned above, there are several other risk factors that increase the likelihood of developing varicose veins and experiencing pain. These include:
1. Age:
As you get older, the valves in your veins may become weaker, making it easier for blood to flow backward and pool in the veins.
2. Gender:
Women are more likely to develop varicose veins than men, likely due to hormonal factors and pregnancy.
3. Family history:
If your parents or other family members have varicose veins, you are more likely to develop them as well.
4. Obesity:
Excess weight puts additional pressure on the veins, increasing the risk of varicose veins and associated pain.
5. Lack of movement:
Leading a sedentary lifestyle and not getting enough exercise can contribute to poor blood circulation and increase the risk of varicose veins.
Common symptoms of varicose vein pain
Varicose vein pain can manifest in different ways, depending on the severity of the condition. Common symptoms include:
1. Aching or throbbing pain in the legs, particularly after prolonged periods of standing or sitting.
2. Swelling and heaviness in the legs, especially towards the end of the day.
3. Itching or irritation around the affected veins.
4. Muscle cramps or a feeling of restless legs.
5. Skin discoloration or the development of ulcers in severe cases.
If you experience any of these symptoms, it is essential to seek medical attention for a proper diagnosis and treatment plan.
Diagnosing varicose veins and determining the underlying cause
To diagnose varicose veins and determine the underlying cause of the pain, a healthcare professional will typically perform a physical examination and may order additional tests. These tests may include:
1. Doppler ultrasound: This non-invasive test uses sound waves to create images of the veins in your legs. It can help identify any abnormalities in blood flow and determine the location and severity of varicose veins.
2. Venogram: In this procedure, a dye is injected into the veins, and X-ray images are taken. It allows the doctor to visualize the flow of blood and identify any blockages or abnormalities.
3. Magnetic resonance imaging (MRI) or computed tomography (CT) scan: These imaging tests may be used in more complex cases to get a detailed view of the veins and surrounding tissues.
Once the cause of varicose vein pain is identified, appropriate treatment options can be explored.
Treatment options for varicose vein pain
The treatment for varicose vein pain depends on the severity of the condition and the underlying cause. Some common treatment options include:
1. Compression stockings: These specially designed stockings apply pressure to the legs, helping to improve blood flow and reduce pain and swelling.
2. Lifestyle modifications: Making certain changes in your daily routine can help alleviate varicose vein pain. Elevating your legs, avoiding prolonged periods of standing or sitting, and regular exercise can all improve blood circulation and reduce discomfort.
3. Sclerotherapy: This minimally invasive procedure involves injecting a solution into the affected veins, causing them to collapse and fade away over time.
4. Endovenous laser treatment (EVLT): In this procedure, a laser is used to heat and seal off the affected veins, redirecting the blood flow to healthier veins.
5. Radiofrequency ablation: Similar to EVLT, radiofrequency ablation uses heat to close off the damaged veins and redirect blood flow.
In more severe cases or when conservative treatments are not effective, surgical interventions such as vein stripping or ligation may be considered. These procedures involve removing or tying off the affected veins to restore proper blood flow.
Lifestyle changes and self-care tips for managing varicose vein pain
In addition to medical treatments, there are several lifestyle changes and self-care tips that can help manage varicose vein pain. These include:
1. Regular exercise: Engaging in activities that promote leg movement, such as walking, swimming, or cycling, can improve blood circulation and reduce pain.
2. Weight management: Maintaining a healthy weight can help alleviate pressure on the veins and reduce the risk of varicose veins.
3. Avoiding tight clothing: Wearing tight-fitting clothes, especially around the waist and legs, can restrict blood flow and exacerbate varicose vein pain.
4. Elevating the legs: Elevating your legs above the heart level for 15-20 minutes several times a day can help reduce swelling and relieve pain.
5. Avoiding high heels: Opting for comfortable shoes with low heels can promote better blood circulation and reduce strain on the legs.
By incorporating these self-care practices into your daily routine, you can effectively manage varicose vein pain and improve your overall well-being.

Preventing varicose veins and reducing the risk of pain
While varicose veins may be unavoidable for some individuals due to genetic factors or other underlying causes, there are measures you can take to reduce the risk of developing them and experiencing pain. These preventive measures include:
1. Regular exercise: Engaging in regular physical activity can help improve blood circulation and strengthen the veins.
2. Maintaining a healthy weight: By maintaining a healthy weight, you can reduce the strain on your veins and lower the risk of varicose veins.
3. Avoiding prolonged periods of standing or sitting: If your job requires long hours of standing or sitting, try to take breaks and engage in leg exercises to promote blood flow.
4. Wearing compression stockings: If you are at a higher risk of developing varicose veins, wearing compression stockings can help support the veins and prevent blood pooling.
5. Elevating the legs: Elevating your legs whenever possible can help reduce the pressure on the veins and promote better blood circulation.
By adopting these preventive measures, you can minimize the likelihood of developing varicose veins and experiencing associated pain.
Seeking professional help for varicose vein pain
If you are experiencing varicose vein pain that is significantly impacting your quality of life, it is crucial to seek professional help. A healthcare professional specialising in vascular conditions, such as phlebologists and vascular surgeons, can provide a proper diagnosis and recommend the most appropriate treatment options for your specific situation.
Remember, you don’t have to suffer in silence. With the advancements in medical technology and the wide range of treatment options available, relief from varicose vein pain is possible.
Conclusion: Empowering individuals to take control of their varicose vein pain journey
Varicose vein pain can be a source of discomfort and frustration for many individuals. However, by understanding the causes of varicose vein pain, recognising the risk factors, and exploring effective treatment options, you can take control of your varicose vein pain journey.
From lifestyle modifications to medical interventions, there are various approaches to managing varicose vein pain. By incorporating self-care practices, seeking professional help when needed, and taking preventive measures, you can alleviate discomfort and improve your overall quality of life.
No more suffering in silence. Empower yourself with knowledge and proactive steps to find relief from varicose vein pain. You deserve to live a life free from the constraints of discomfort and enjoy the activities you love with confidence and ease.