Table of Contents
Venous thromboembolism (VTE) refers to the formation of blood clots in the veins, most commonly occurring in the legs or pelvis. It encompasses two main conditions: deep vein thrombosis (DVT) and pulmonary embolism (PE). DVT involves the formation of blood clots in deep veins, while PE occurs when a clot dislodges from a vein and travels to the lungs, potentially causing a blockage. VTE can be a serious and sometimes life-threatening condition, but with prompt diagnosis and appropriate treatment, the risks can be minimised.
What is Venous Thromboembolism?
Venous thromboembolism (VTE) refers to a condition where blood clots form within a blood vessel , block the blood flow and can potentially dislodge, travelling through the bloodstream and causing blockages in other parts of the body. Venous thromboembolism (VTE) typically occurs in the deep veins of the legs, called deep vein thrombosis (DVT), but it can also affect veins in other areas such as the arms or pelvis. If a blood clot breaks free and reaches the lungs, it can result in a life-threatening condition called pulmonary embolism (PE).
Venous thromboembolism (VTE) is primarily caused by a combination of factors known as Virchow’s triad:
1. Venous Stasis:
Slow or impaired blood flow within the veins, often due to inactivity, prolonged bed rest, or immobilisation after major surgery or injury.
2. Hypercoagulability:
Increased tendency of the blood to clot, which can be caused by certain medical conditions (such as cancer or genetic clotting disorders), hormonal changes (such as pregnancy or use of hormone therapy), or medication.
3. Endothelial Injury:
Damage to the inner lining of a blood vessel, which can result from trauma, surgery, inflammation, or underlying medical conditions.
Symptoms of Venous thromboembolism (VTE) can vary depending on the location and severity of the blood clot. Common signs and symptoms include swelling, pain, warmth, and redness in the affected area. In the case of pulmonary embolism, symptoms may include sudden shortness of breath, chest pain, coughing up blood, and rapid heartbeat.
Risk Factors for DVT
Several risk factors can increase the venous thromboembolism risk. It’s important to note that having one or more risk factors doesn’t necessarily mean a person will develop DVT, but it’s important to be aware of these factors. The main risk factors for DVT include:
1. Prolonged immobility
Extended periods of immobility, such as during long-distance travel, bed rest, or hospitalisation, can increase the risk of DVT. The lack of movement slows down blood flow, making it easier for blood clots to form.
2. Surgery
Surgical procedures are a risk factor, especially those involving the lower extremities, pelvis, or abdomen, can increase the risk of DVT. The trauma to blood vessels during surgery and the postoperative immobility contribute to clot formation.
3. Trauma or injury
Injuries that damage blood vessels or cause significant tissue damage are a risk factor of blood clots. This includes fractures, severe muscle injuries, or major trauma in hospitalised patients.
4. Cancer and cancer treatments
Some types of cancer, particularly pancreatic, lung, and haematologic cancers, increase the risk of blood clots. Additionally, certain cancer treatments like chemotherapy can affect blood clotting factors.
5. Hormonal factors
Hormonal changes can affect blood clotting. Women who take oral contraceptives or hormone replacement therapy (HRT), especially those containing oestrogen, have a slightly higher risk of developing DVT.
6. Pregnancy and postpartum period
Pregnancy increases the risk of blood clots due to hormonal changes, increased pressure on veins, and reduced blood flow in the legs. The risk continues for about six weeks after giving birth.
7. Obesity
Being overweight or obese puts extra pressure on the veins and can hinder blood flow, increasing the the risk factor of clot formation.
8. Age
The risk of DVT increases with age. While DVT can occur at any age, it is more common in individuals over 60.
9. Inherited or acquired blood clotting disorders
Certain genetic conditions that affect blood clotting, such as factor V Leiden mutation or deficiencies in proteins C and S, can increase the risk of DVT. There is often a family history of deep vein thrombosis. Additionally, acquired clotting disorders, such as antiphospholipid syndrome, can also increase the risk.
10. Previous history of DVT or pulmonary embolism
Individuals who have experienced DVT or pulmonary embolism in the past have an increased risk of recurrence.
11. Other medical conditions
Certain medical conditions, such as heart failure, inflammatory bowel disease such as Crohn’s disease, chronic kidney disease, and varicose veins, can increase the risk of DVT.
How does deep venous thrombosis occur?
Venous thromboembolic disease occurs when a blood clot forms within a vein, typically in the deep veins of the legs (known as deep vein thrombosis or DVT), and can potentially dislodge, travel through the bloodstream, and cause blockages in other parts of the body. Here’s an overview of how Venous thromboembolism occurs:
1. Virchow’s Triad:
The development of VTE is often associated with factors known as Virchow’s triad, which includes three main components:
a. Venous Stasis: Slow or impaired blood flow within the veins is one of the key factors in clot formation. Venous stasis can occur due to factors such as immobility, prolonged bed rest, long-distance travel, or conditions that restrict the normal flow of blood.
b. Hypercoagulability: Hypercoagulability refers to an increased tendency of the blood to clot. Various factors contribute to this, including genetic conditions (such as factor V Leiden mutation or deficiencies in proteins C and S), certain medications (such as hormone replacement therapy or birth control pills containing oestrogen), cancer, pregnancy, or autoimmune disorders.
c. Endothelial Injury: Damage to the inner lining of the blood vessels, called the endothelium, can trigger the formation of blood clots. Injury to the endothelium can occur due to trauma, surgery, inflammation, or underlying medical conditions.
2. Blood Clot Formation:
When there is a disruption in the balance between blood coagulation (clotting) and anticoagulation (preventing clots), it can lead to the formation of a blood clot. The clot typically develops in a deep vein, most commonly in the lower leg or thigh.
3. Clot Propagation and Embolization:
If the blood clot continues to grow or becomes unstable, it may partially or completely block the flow of blood into the affected vein. In some cases, a portion of the clot can break off and travel through the bloodstream. This is known as an embolus. If the embolus reaches the lungs, it can cause a blockage known as a pulmonary embolism (PE), which can be life-threatening.
It’s important to note that not all individuals with risk factors for VTE will develop blood clots, and some cases may occur without any identifiable risk factors. However, understanding the factors that contribute to VTE can help in identifying individuals at higher risk and implementing preventive measures to reduce the likelihood of clot formation.
Complications of DVT
Deep vein thrombosis (DVT) can lead to several complications, some of which can be serious or life-threatening if left untreated. It’s important to recognise these potential complications and seek prompt medical attention. Here are some common complications associated with DVT:
1. Pulmonary Embolism (PE)
The most serious complication of DVT is when a blood clot dislodges from the vein and travels to the lungs, causing a blockage known as pulmonary embolism. PE can impair blood flow to the lungs and lead to symptoms such as sudden shortness of breath, chest pain, rapid breathing, coughing up blood, and even cardiac arrest or death.
2. Post-Thrombotic Syndrome (PTS)
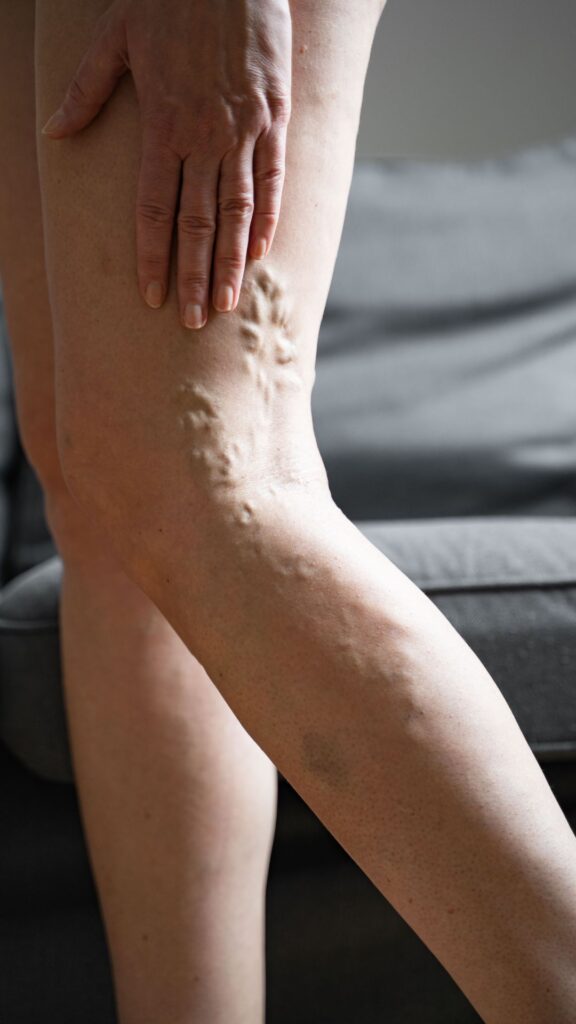
After a DVT episode, some individuals may develop post-thrombotic syndrome. This condition can cause long-term complications and symptoms such as chronic leg pain, swelling, heaviness, skin discoloration, and ulcers. It occurs due to damage to the veins and impaired blood flow resulting from the previous blood clot.
3. Recurrent DVT
Individuals who have experienced DVT once are at a higher risk of developing another episode in the future. The risk of recurrence can vary based on factors such as the underlying cause of the initial DVT, the presence of certain genetic or acquired clotting disorders, and the effectiveness of preventive measures taken.
4. Chronic Venous Insufficiency (CVI)
DVT can damage the valves in the veins, leading to a condition called chronic venous insufficiency. CVI causes impaired or slow the flow of blood even in the affected veins, resulting in symptoms such as swelling, pain, varicose veins, skin changes, and leg ulcers.
5. Venous Gangrene
In rare cases, severe DVT can lead to a condition called venous gangrene, which is characterised by tissue death (necrosis) in the affected limb. Venous gangrene requires immediate medical attention and often requires surgical intervention.
6. Paradoxical Embolism
Paradoxical embolism occurs when a blood clot from the veins crosses over to the arterial circulation through an abnormal connection between the right and left sides of the heart (such as a patent foramen ovale). This can lead to strokes or other arterial blockages.
7. Death
Although less common, untreated or severe cases of DVT can result in death, particularly if a large pulmonary embolism occurs or if complications lead to organ failure.

What tests are used to diagnose venous thromboembolism?
Several tests can be used to diagnose venous thromboembolism (VTE). The choice of tests depends on the individual’s symptoms, clinical presentation, and the healthcare provider’s judgment. Here are some common diagnostic tests for VTE:
1. D-Dimer Test
The blood test called D-dimer measures the levels of a protein fragment produced when blood clots are broken down. A positive D-dimer result suggests the presence of a clot but does not indicate its location or size. This blood is often used as a screening tool to rule out VTE in individuals with a low pre-test probability.
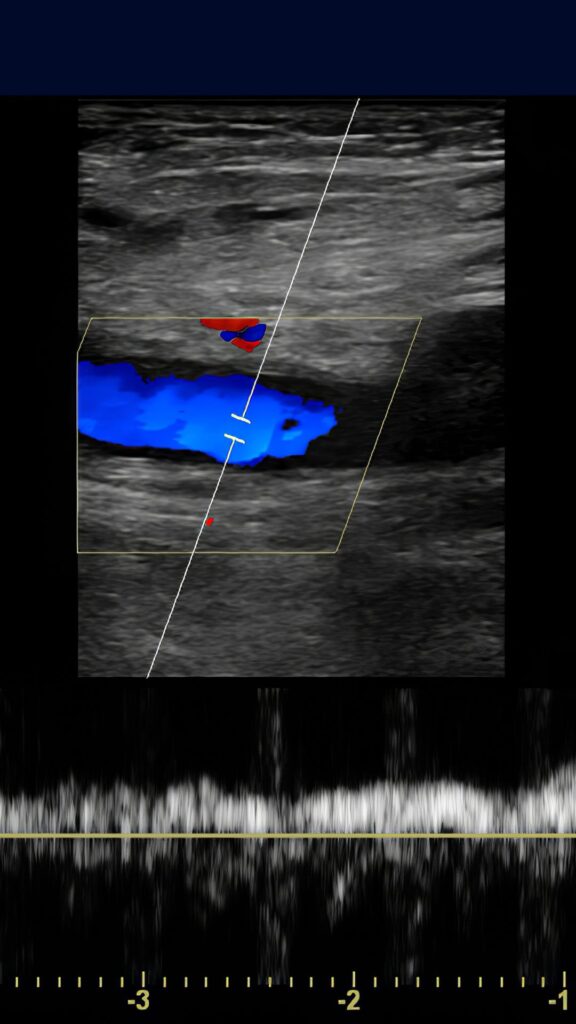
2. Compression Ultrasound (Duplex Ultrasound)
This imaging test uses sound waves to visualise blood flow in the veins. It is commonly performed to detect deep vein thrombosis (DVT) in the legs. During the test, a technologist applies pressure with an ultrasound probe to compress the veins to detect blood clots and assess for the presence of a clot.
3. Venography
Venography involves injecting a contrast dye into a vein, usually in the foot or ankle, and taking X-ray images to visualise the veins. This test is more invasive and is typically reserved for cases where other diagnostic methods are inconclusive.
4. CT Scan (Computed Tomography)
CT scan can be used to diagnose both deep vein thrombosis (DVT) and pulmonary embolism (PE). In a CT venography, a contrast dye is injected, and a series of X-ray images are taken to visualise the veins. A CT pulmonary angiogram (CTPA) involves imaging of the pulmonary arteries to identify blood clots in the lungs.
5. Blood Tests
In some cases, blood tests may be performed to assess specific clotting disorders or abnormalities that contribute to VTE risk, such as genetic mutations or deficiencies in clotting factors.
How Do you Treat Venous Thromboembolism?
Treatment for VTE typically involves the use of anticoagulant medications or blood thinners, to prevent the clot from growing and to reduce the risk of further clotting. In some cases, more invasive treatments such as thrombolytic therapy (to dissolve the clot) or surgical interventions may be necessary.
Venous thromboembolism prevention involves early mobilisation after surgery or extended periods of inactivity, maintaining a healthy weight, regular exercise, wearing compression stockings, and taking appropriate preventive measures (such as blood thinners medication) in high-risk situations.
When to see a doctor
It is important to seek medical care if you experience any signs or symptoms that may suggest the presence of venous thromboembolism (VTE). These include unexplained leg swelling, leg pain or tenderness, difficulty breathing or chest pain, history of VTE or known risk factors, concerns about medications or treatments, and recurrent or persistent symptoms. Early detection and appropriate treatment of VTE can significantly reduce the risk of complications. If you suspect you may have VTE or are uncertain about your symptoms, it is best to err on the side of caution and consult a healthcare professional promptly. They can assess your situation, perform any necessary tests, and provide the appropriate guidance and treatment.