What is the sclerotherapy procedure like?
Sclerotherapy is a minimally invasive procedure used to treat varicose and spider veins, primarily on the legs. It involves the injection of a sclerosing agent directly into the affected veins, causing them to shrink, collapse, and eventually fade away or become less visible. The procedure is popular due to its effectiveness, minimal discomfort, and relatively quick recovery time. Here’s what the sclerotherapy procedure typically involves:
Before the Procedure
– Consultation: Initially, you’ll have a consultation with a vein doctor to assess your veins and discuss the best treatment approach. This may include a physical examination and possibly an ultrasound scan to evaluate the vein’s size and blood flow.
– Preparation: You may be advised to avoid certain medications, such as aspirin or ibuprofen, and to refrain from applying lotion to the legs before the procedure.
During the Procedure
– Environment: Sclerotherapy is usually performed in a doctor’s office and does not require anaesthesia. The procedure typically takes 30 minutes to an hour, depending on the number of veins being treated.
– Process: You will lie on your back with your legs slightly elevated. The doctor will clean the treatment area and then use a fine needle to inject the sclerosing solution into the targeted veins. You might feel minor stings or cramps when the needle is inserted.
– Mechanism: The injected solution causes irritation to the lining of the vein, leading to its collapse. Over time, the treated vein turns into scar tissue and gradually fades from view. In some cases, foam sclerotherapy may be used, especially for larger veins. This involves turning the sclerosing agent into a foam before injection into enlarged veins, allowing it to cover a larger surface area within the vein.
After the Procedure
– Immediate Care: After the injections, compression stockings or bandages are applied to the treated areas to maintain pressure on the veins, help reduce bruising, and enhance the effectiveness of the treatment.
– Recovery: There’s little to no downtime, and most patients can return to their normal activities the same day, though strenuous exercise should be avoided for a couple of days. Walking is encouraged to promote blood flow.
– Follow-Up: You may need several sclerotherapy sessions, depending on the number and size of veins being treated. Follow-up treatments are usually scheduled every 4 to 6 weeks.
Results and Expectations
– Visibility: It typically takes a few weeks to months for the spider veins treated to fade completely. Smaller veins usually respond to treatment in 3 to 6 weeks, while larger veins may take 3 to 4 months.
– Effectiveness: While sclerotherapy is effective for most patients, it does not prevent new varicose or spider veins from emerging. Future treatments may be necessary to maintain results.
– Side Effects: Common side effects include bruising, redness, and swelling at the injection site, but these usually subside within a few days. More rare complications can include inflammation, small skin ulcers, or the formation of small blood clots.
Sclerotherapy is considered a safe and effective treatment for reducing the appearance of varicose and spider veins. If you’re considering this procedure, consult with a vein specialist to discuss your suitability for sclerotherapy and what you can expect from the treatment.
What causes varicose veins and other diseased vein types to become visible?
Varicose veins and other types of diseased veins become visible due to a combination of factors that affect the circulation and health of the veins. These factors lead to the enlargement and malfunctioning of the veins, making them prominent under the skin. Here are the primary reasons why these abnormal veins become visible:
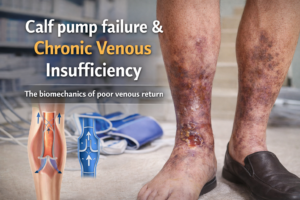
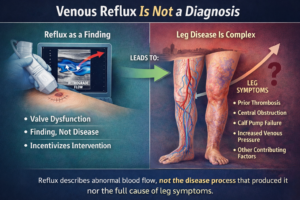
1. Valve Failure: The veins in your legs have one-way valves that help blood travel back up to the heart against gravity. When these valves become weak or damaged, they fail to close the blood flowing back properly, allowing blood to flow backward and pool in the vein. This pooling causes the vein to become enlarged and varicose.
2. Venous Insufficiency: This condition occurs when your veins have trouble sending blood from your limbs back to the heart. It’s often caused by valve failure and can lead to varicose veins. Chronic venous disease can result in increased pressure within the veins, further a blood clot and exacerbating the visibility and severity of varicose veins.
3. Blood Pressure Increase: When valves are not working properly, the pressure within the vein increases. This, increased blood volume and pressure can cause the vein to become enlarged, stretched, and twisted, making them more visible under the skin.
4. Age: As you age, your veins can lose elasticity, causing them to stretch. The valves in your veins may also weaken over time, increasing the risk of valve failure and the development of varicose veins.
5. Hormonal Changes: Hormonal changes associated with puberty, pregnancy, and menopause can relax the walls of the veins, contributing to the development of varicose veins. During pregnancy, the increase in the volume of blood can also add pressure to the veins.
6. Lifestyle and Occupation: Prolonged standing or sitting can contribute to the development of varicose veins due to increased pressure in the veins of your lower body. A sedentary lifestyle can also contribute to weakened veins and poor circulation.
7. Obesity: Carrying extra weight puts additional pressure on your veins, which can lead to valve failure and the formation of varicose veins.
8. Genetics: A family history of varicose veins can increase your risk of developing them. If other family members have had varicose veins or other vein problems, you’re more likely to have them as well.
These factors contribute to the weakening of vein walls and valve malfunction, leading to the pooling of blood. As a result, veins can become enlarged, twisted, and visible under the surface of the skin, often appearing blue or dark purple.
Are spider veins caused by poor circulation?
Yes, spider veins can be caused by poor circulation, among other factors. Spider veins, also known as telangiectasias, are small, dilated blood vessels that appear close to the surface of the skin and often look like spider webs or branches. They are smaller than varicose veins and are usually red, purple, or blue. While they can occur anywhere on the body, they are most commonly found on the legs and face.
Poor circulation contributes to the development of spider veins by increasing pressure trapped blood from within the veins. This pressure can result from various factors, including prolonged standing or sitting, which hinders the normal flow of blood back to the heart and causes blood to pool in the veins. Over time, this increased pressure can weaken the blood vessel walls, leading to the formation of spider veins.
Other factors that can contribute to the development of spider veins include:
– Hormonal changes: Hormonal fluctuations associated with puberty, pregnancy, menopause, and the use of hormonal birth control or hormone replacement therapy can increase the risk of spider veins. Hormones can affect the elasticity and valve functioning in veins, leading to weakened vessels.
– Age: As you age, your veins lose elasticity, and the valves in your veins may weaken, making it harder for them to prevent the backflow of blood. This can increase the likelihood of spider and varicose veins.
– Genetics: A family history of spider or varicose veins can increase your risk of developing them.
– Obesity: Extra weight puts additional pressure on your veins, which can lead to the development of spider veins.
– Sun exposure: Sun damage, especially on the face, can lead to the breaking of small blood vessels and the appearance of spider veins.
While poor circulation is a contributing factor to spider veins, it’s important to note that a combination of factors usually leads to their development. Managing risk factors, when possible, may help prevent or reduce the severity of spider veins.
What treatments are available to remove dilated blood vessels in the legs?
To address and remove dilated blood vessels in the legs, including varicose and spider veins, several effective treatments are available. These treatments range from minimally invasive procedures to more traditional surgical options, depending on the severity and type of vein issue. Here’s an overview of the most common treatments:
1. Sclerotherapy
This is a popular treatment for both spider veins and smaller varicose veins. A solution, usually a saline or a specially formulated chemical, is injected directly into the vein. This causes the vein to scar and collapse, forcing blood to reroute through healthier veins. The collapsed vein is reabsorbed into local tissue and eventually fades.
2. Laser Treatments
– Simple Laser Treatment: This is performed on the surface of the skin, treating spider veins and small varicose veins just under the skin’s surface. Multiple laser treatment sessions are often required.
– Endovenous Laser Treatment (EVLA): Used for varicose veins in the legs, a laser fiber is passed through a catheter into the vein, using laser energy to seal it off.
3. Radiofrequency Ablation (RFA)
Similar to EVLT, this method uses radiofrequency energy instead of laser energy to heat up and damage the wall inside a varicose vein, causing it to collapse and seal shut. This procedure is also used for larger varicose veins.
4. Endoscopic Vein Surgery
For severe cases, especially when there’s a risk of leg ulcers, this minimally invasive surgery involves the insertion of a thin video camera into the vein to visualise and close varicose veins, then remove them through small incisions. This is typically considered only when other treatments have failed.
5. Ambulatory Phlebectomy
Small varicose veins are removed through a series of tiny skin punctures. Only the parts of your leg that are being pricked are numbed in this outpatient procedure. This treatment is effective for removing superficial treat varicose veins, and offers minimal downtime.
6. Vein Stripping and Ligation
This is a surgical procedure that involves tying off a vein before it joins a deep vein and removing the vein through small incisions. This is less commonly performed now due to more effective, less invasive treatments being available.
7. Compression Stockings
Wearing compression stockings is often the first approach to try before moving on to other treatments. They steadily squeeze your legs, helping veins and leg muscles move blood more efficiently. While they don’t remove veins, they can help alleviate symptoms and slow the progression of vein disease.
8. Lifestyle Changes
For managing mild symptoms and preventing the progression of vein issues, lifestyle changes such as regular exercise, maintaining a healthy weight, elevating the legs, and avoiding long periods of standing or sitting can be beneficial.
Choosing the right treatment depends on various factors, including the severity and type of vein problem, your general health, and your personal preferences. A consultation with a vein specialist or vascular surgeon is essential to determine the most appropriate treatment plan for your specific vein condition alone.
When can I resume my sporting activities after treatment?
Resuming sporting activities after vein treatment depends on the specific procedure you’ve undergone and your individual recovery process. It’s crucial to follow the guidelines provided by your healthcare provider, as they will tailor advice based on the details of your treatment and personal health profile. Here’s a general overview of when you might expect to return to sports after common vein treatments:
Sclerotherapy
– Light exercise: Can usually be resumed immediately or within a few days, encouraging walking to promote circulation.
– Strenuous activities: It’s often recommended to wait 1 to 2 weeks before engaging in high-impact sports or intense workouts.
Laser Treatments
– Simple laser treatments: Normal activities can typically be resumed the same day, but strenuous exercise should be avoided for 1 to 2 weeks.
– Endovenous laser treatment (EVLT): A recovery period of 1 to 2 weeks is generally advised before returning to vigorous physical activities.
Radiofrequency Ablation (RFA)
– Light activities: Walking and light daily tasks are encouraged almost immediately after the procedure.
– High-impact sports: Similar to EVLT, waiting for 1 to 2 weeks is advisable before resuming strenuous exercises.
Endoscopic Vein Surgery
– Recovery period: Given the invasive nature of the surgery, you may need to limit physical activity for 2 to 4 weeks, with a gradual return to more intense activities.
Ambulatory Phlebectomy
– Light exercise: Can often be resumed quickly, within a few days post-procedure.
– Strenuous exercise: Generally, it’s best to wait 1 to 2 weeks before undertaking high-impact sports.
Vein Stripping and Ligation of Varicose Vein
– Recovery time: This surgical option requires a longer recovery, potentially 2 to 4 weeks for light exercise and longer for intensive sports activities.
Key Considerations:
– Follow Post-Treatment Instructions: Adhering to your healthcare provider’s specific recommendations is crucial for a successful recovery.
– Wear Compression Stockings: If prescribed, wearing compression stockings as directed can support your recovery and improve treatment outcomes.
– Listen to Your Body: Ease back into your sporting activities gradually, and be attentive to any signs of discomfort or swelling. If you encounter any issues, pause your activities and consult your healthcare provider.
Remember, these timelines are general guidelines, and your specific situation may vary. Always prioritize the advice given by your vein doctor, as they understand the nuances of your treatment and recovery needs best.
Can spider veins and varicose veins return after treatment?
Yes, spider veins and varicose veins can return after treatment. While the current treated veins are usually eliminated effectively, the treatments do not prevent the formation of new varicose or spider veins in the future. Several risk factors contribute to the potential recurrence or appearance of new veins, including:
1. Genetic Predisposition: If you have a family history of varicose or spider veins, you may be more prone to developing them, regardless of treatment.
2. Underlying Venous Insufficiency: Treatments like sclerotherapy or laser therapy remove or close the visible veins but might not cure the underlying venous disease. Without addressing the root cause, new varicose or spider veins can develop in different areas.
3. Lifestyle and Health Factors: Conditions such as obesity, a sedentary lifestyle, and occupations requiring prolonged standing or sitting can increase the pressure in the leg veins, leading to the development of new varicose or spider veins.
4. Hormonal Changes: Hormonal fluctuations associated with pregnancy, menopause, and the use of hormonal birth control or hormone replacement therapy can affect vein health and lead to the development of new veins.
5. Aging: As you age, the risk of developing varicose and spider veins increases due to the natural loss of vein elasticity and weakening of vein valves.
To minimize the risk of recurrence or the development of new varicose or spider veins, it’s important to address the underlying causes as much as possible and adopt preventive measures. Some strategies include:
– Exercise regularly to improve blood circulation and muscle tone.
– Maintain a healthy weight to reduce pressure on your veins.
– Elevate your legs when resting to improve circulation.
– Avoid prolonged periods of standing or sitting. If your job requires it, try to move around or change positions frequently.
– Wear compression stockings, especially if you are prone to varicose or spider veins, as they can help improve blood flow and decrease pressure in the veins.
– Follow-up care: Regular check-ups with a vein specialist can help monitor your vein health and address any new issues early on.
While some treatment options can significantly reduce the appearance and symptoms of varicose and spider veins, understanding the potential for new veins to develop and taking preventive steps can help manage your vein health over the long term.
Does laser and sclerotherapy hurt?
Laser treatments and sclerotherapy for varicose and spider veins are generally well-tolerated, but patients may experience some discomfort during and after the procedures. The level of pain or discomfort can vary depending on the individual’s pain threshold, the extent of the treatment, and the specific technique used. Here’s what you can expect from each treatment:
Laser Treatments
During the Procedure:
– Laser treatments involve delivering bursts of light energy to the vein walls, which can feel like a rubber band snapping against the skin. Most modern laser systems have cooling devices or use techniques to minimize discomfort during the procedure.
– The sensation is generally quick and may be followed by a brief period of warmth or tingling in the treated area.
After the Procedure:
– Post-treatment, the area may feel tender or swollen for a few days. Over-the-counter pain relievers and cold compresses can help alleviate any discomfort.
– Some patients report a sensation of tightness or cramping in the treated area for a short period after the procedure.
Sclerotherapy
During the Procedure:
– Sclerotherapy involves injecting a solution directly into the vein, which can cause mild discomfort or a burning sensation for a few minutes, especially when larger veins are treated.
– The discomfort is typically short-lived, and the procedure itself takes only about 15 to 30 minutes, depending on the number of veins being treated.
After the Procedure:
– After sclerotherapy, it’s common to experience some bruising, redness, or minor soreness at the injection sites. These symptoms usually resolve within a few days to a few weeks.
– Some patients may feel a slight itching or have tender lumps in the veins that has been treated, which indicates the treatment is working. This can last for a few days to several weeks.
Managing Discomfort for the Treatment of Leg Veins
Both laser treatments and sclerotherapy are outpatient procedures, and most patients can resume their normal activities shortly after. To manage any discomfort, healthcare providers may recommend the following:
– Wearing compression stockings to improve circulation and reduce soreness.
– Over-the-counter pain relievers, such as acetaminophen or ibuprofen, to alleviate pain.
– Avoiding strenuous exercise or high-impact activities for a few days following treatment to allow the treated area to heal.
It’s important to discuss any concerns about pain or discomfort with your healthcare provider before undergoing treatment. They can provide more detailed information on what to expect based on your specific situation and may offer additional strategies to ensure your comfort during and after the procedure.