Navigating through the complexities of Nutcracker Syndrome can be a daunting task for patients and their loved ones. This rare vascular disorder affects the blood flow in the abdomen and pelvis, causing a range of distressing symptoms. From debilitating pain and blood in urine to varicocele and fertility issues, Nutcracker Syndrome can significantly impact the quality of life of those affected.
In this article, we delve into the depths of Nutcracker Syndrome, shedding light on its causes, symptoms, and available treatment options. Through a comprehensive understanding of this condition and medical history, patients and their loved ones can gain the knowledge needed to make informed decisions about healthcare and support.
Moreover, we explore the importance of emotional and mental support for patients and their families, as developing Nutcracker Syndrome often poses unique challenges that extend beyond the physical symptoms. By providing valuable insights and resources, we aim to empower individuals affected by Nutcracker Syndrome to seek the help they need, find solace in supportive networks, and ultimately enhance their overall well-being.
What is Nutcracker Syndrome?
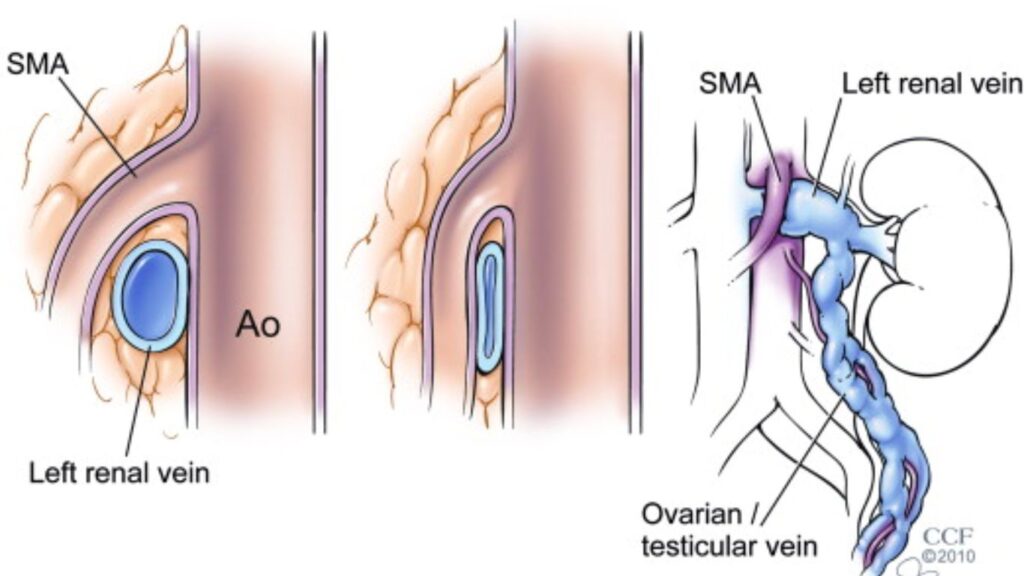
Nutcracker Syndrome is a rare vascular disorder that occurs when the left renal vein, which carries blood away from the left kidney, becomes compressed between the aorta and the superior mesenteric artery. This compression leads to a disruption in blood flow, causing a variety of symptoms. While the nutcracker syndrome surgery primarily affects the left renal vein, it can also impact other nearby structures, such as the ureter and testicular veins
What Causes This Renal Vein Entrapment Syndrome?
Nutcracker syndrome’s primary cause lies in the anatomical compression of the left renal vein. The compression results in increased pressure in the vein, leading to blood flow disturbances and subsequent symptoms.
Left Renal vein Anatomy of Nutcracker Syndrome
In Nutcracker syndrome, the left renal vein (LRV) experiences compression between two major blood vessels: the abdominal aorta and the superior mesenteric artery. This compression leads to various symptoms due to restricted blood flow within the left side renal veins and vein transposition itself.
1. Abdominal Aorta:
– The abdominal aorta is the large artery that descends from the thoracic (chest) aorta into the abdominal cavity. It supplies oxygenated blood to various abdominal organs, including the kidneys.
2. Superior Mesenteric Artery (SMA):
– The superior mesenteric artery is a major blood vessel arising from the abdominal aorta. It provides blood supply to the small intestine and part of the large intestine.
3. Left Renal Vein (LRV):
– The left renal vein is the vein that carries blood away from the left kidney. It usually runs between the abdominal aorta and the superior mesenteric artery, and in Nutcracker syndrome, it gets compressed between these two vessels.
Symptoms of Nutcracker Syndrome
The symptoms of Nutcracker Syndrome can vary from person to person, and some individuals may experience more severe symptoms than others. Common symptoms renal nutcracker syndrome include chronic abdominal pain, particularly in the left flank, blood in urine, varicocele (enlarged veins in the scrotum), and pelvic congestion syndrome. In some cases, Nutcracker Syndrome can also lead to fertility issues, as the disrupted blood flow can impact the health and function of the reproductive organs.
Nutcracker Syndrome vs Nutcracker Phenomenon
Nutcracker syndrome and Nutcracker phenomenon are related conditions, but they involve distinct aspects of vascular compression and can differ in their presentation and severity.
Nutcracker Syndrome:
Cause: Nutcracker syndrome is a vascular compression disorder where the left renal vein is compressed between the abdominal aorta and the superior mesenteric artery, leading to symptoms and potential complications due to blood flow obstruction.
Symptoms: Common symptoms of Nutcracker syndrome include hematuria (blood in urine), flank pain, abdominal pain, varicocele (enlarged veins in the scrotum, mainly in males), and proteinuria (protein in urine).
Diagnosis and Treatment: Diagnosis involves imaging tests such as Doppler ultrasound, CT scans, or MRI to visualize the compression and assess blood flow. Treatment options may include conservative management, interventional procedures (such as stenting or embolization), or in severe cases, surgical intervention.
Nutcracker Phenomenon:
Definition: Nutcracker phenomenon refers to the anatomical compression of the left renal vein without the development of significant clinical symptoms or complications. In this case, the compression might be present, but the individual may not exhibit noticeable or unusual clinical manifestations.
Asymptomatic Compression: Unlike Nutcracker syndrome, individuals with Nutcracker phenomenon might not experience significant symptoms or complications despite the vascular compression of the left renal vein.
Observation: Diagnosis of Nutcracker phenomenon might occur incidentally during imaging studies performed for other reasons, and it may not require active treatment if the individual remains asymptomatic.
Conclusion
While both Nutcracker syndrome and Nutcracker phenomenon involve the compression of the left renal vein, Nutcracker syndrome manifests as severe pain with notable symptoms and potential complications, whereas Nutcracker phenomenon refers to the compression without significant clinical impact. Proper diagnosis and differentiation between these conditions are crucial for determining appropriate management strategies tailored to the individual’s specific symptoms and needs.
Diagnosing Nutcracker Syndrome
Diagnosing Nutcracker Syndrome can be challenging, as its symptoms can overlap with those of other conditions. However, there are several diagnostic tools that healthcare professionals can use to identify the and diagnose nutcracker syndrome well. These include imaging tests such as ultrasound, computed tomography (CT) scan, magnetic resonance imaging (MRI), and venography.
During these tests, the healthcare provider will look for signs of compression or narrowing in the left renal vein. They may also measure the pressure in the left renal vein to determine the severity of the condition. Additionally, the healthcare provider may perform a urine analysis and blood tests to rule out other potential causes of the symptoms.
Ultrasound Assessment of Nutcracker Syndrome
Ultrasound assessment plays a pivotal role in diagnosing Nutcracker syndrome, offering a non-invasive and readily available method to visualise the compression of the left renal vein. Here’s how ultrasound is used in assessing Nutcracker syndrome:
Doppler Ultrasound Examination:
1. Visualization of Vascular Anatomy:
– Ultrasound allows visualization of the abdominal structures, including the abdominal aorta, superior mesenteric artery, and the left renal vein. It helps in assessing the anatomical relationship between these vessels.
2. Measurement of Renal Vein Diameter and Flow:
– Doppler ultrasound measures the diameter of the left renal vein and evaluates blood flow patterns within the vein. Compression often leads to changes in the vein’s diameter and altered blood flow dynamics, which can be observed through this imaging technique.
3. Renal Vein Pressure Gradient:
– In some cases, Doppler ultrasound can estimate the pressure gradient across the left renal vein by assessing the velocity of blood flow. A significant pressure gradient can indicate compression and obstruction.
4. Comparison with Respiration:
– Ultrasound can also assess changes in the diameter of the left renal vein during different phases of respiration. The compression might become more evident during certain breathing patterns.
Limitations of Ultrasound:
– Operator Dependence:
The accuracy of ultrasound assessment for Nutcracker syndrome can vary depending on the skill and experience of the ultrasound technician.
– Body Habitus and Patient Positioning:
Some patients’ body types or positions might make it challenging to obtain clear imaging of the left renal vein and its compression.
Confirmatory Tests:
While ultrasound serves as an initial and non-invasive diagnostic tool for Nutcracker syndrome, confirmatory imaging studies such as CT scans, MRI, or venography might be employed for a more detailed assessment, especially in cases where ultrasound results are inconclusive or further clarity is required regarding the severity and anatomical details of the compression.
Conclusion:
Doppler ultrasound remains a valuable and widely used method in the initial evaluation of Nutcracker syndrome due to its non-invasive nature. However, it might be complemented by other imaging modalities for a comprehensive assessment and confirmation of the diagnosis, ensuring appropriate management strategies for individuals affected by this condition.
The link between Nutcracker Syndrome and Pelvic congestion syndrome
Nutcracker syndrome and pelvic congestion syndrome (PCS) both involve venous disorders but affect different vascular regions within the pelvic area, albeit with some potential interrelation.
There can be an association or overlap between Nutcracker syndrome and PCS due to their proximity in the pelvic region and their shared underlying mechanism of venous congestion.
– Shared Venous Insufficiency: Nutcracker syndrome, by causing venous hypertension and venous blood flow disturbances, may contribute to the development or exacerbation of pelvic congestion and the associated varicose veins in the pelvic area.
– Secondary Impact: The increased pressure and altered blood flow dynamics resulting from Nutcracker syndrome could potentially lead to the dilation of pelvic veins, contributing to the manifestation of PCS symptoms.
While Nutcracker syndrome and PCS involve distinct venous territories within the pelvic area, the impact of venous congestion resulting from anterior Nutcracker syndrome might contribute to or exacerbate the symptoms and manifestations of pelvic congestion in posterior nutcracker syndrome itself. Understanding the potential interrelation between these conditions can be crucial in diagnosing and managing patients presenting with pelvic pain and venous-related issues in the pelvic region. Collaboration between specialists in nephrology, urology, and gynaecology may be necessary for comprehensive evaluation and treatment in cases with suspected overlapping conditions.
Does nutcracker syndrome affect the heart?
Nutcracker syndrome primarily involves the compression of the left renal vein, leading to symptoms related to renal impairment and venous congestion in the left kidney and surrounding structures. Generally, Nutcracker syndrome doesn’t directly affect the heart.
However, in rare and severe cases, chronic renal vein compression and resultant venous congestion may potentially lead to certain complications that could indirectly impact the cardiovascular system. These complications may include:
Renal Impairment:
– Hypertension: Nutcracker syndrome might lead to hypertension due to increased renin production resulting from renal ischemia or altered kidney function.
Venous Hypertension:
– Systemic Effects: Chronic venous congestion or hypertension in the left renal vein might impact overall venous circulation, potentially affecting systemic blood pressure regulation.
– Compensatory Mechanisms: The body might activate compensatory mechanisms to manage altered blood flow dynamics, which could indirectly influence cardiovascular function.
– Indirect Effects: While the primary impact of Nutcracker syndrome remains within the renal system, severe and chronic cases might indirectly contribute to systemic effects or alterations that could influence cardiovascular health. However, these occurrences are rare and generally observed in more extreme or prolonged instances of Nutcracker syndrome.
In most cases, Nutcracker syndrome primarily affects the renal system and may lead to localized symptoms related to the compression of the left renal vein. However, severe and chronic cases might potentially lead to complications that could indirectly impact the cardiovascular system, mainly through the effects of chronic venous congestion or altered renal function. These indirect effects, though rare, might have implications for cardiovascular health and blood pressure regulation. Consulting with healthcare providers for comprehensive evaluation and management is crucial in addressing potential systemic effects or complications associated with Nutcracker syndrome.
Is nutcracker syndrome worse lying down?
Nutcracker syndrome symptoms can vary among individuals, and the severity or presentation of symptoms might not always correlate directly with body position, including lying down. However, some individuals might experience variations in symptoms or discomfort in different positions, including when lying down.
– Upright Position: Symptoms such as left flank pain or, hematuria (blood in urine), or varicocele might be more noticeable or exacerbated when standing or in an upright position due to increased pressure on the left renal vein.
– Supine Position (Lying Down): In some cases, lying down might alleviate symptoms or reduce discomfort by minimizing gravitational effects and potentially easing venous congestion in the left renal vein. However, this relief might not be consistent among all individuals with Nutcracker syndrome.
– Individual Variation: Symptoms and their severity can vary significantly among those affected by Nutcracker syndrome. Some individuals may find certain positions more comfortable, while others might not experience significant changes in symptoms based on body position.
While some individuals might experience fluctuations in symptoms, including relief or exacerbation when lying down, there isn’t a consistent pattern observed across all cases of Nutcracker syndrome. Body position and its effect on symptoms can vary among individuals, and the assessment of symptoms in different positions might be part of the overall evaluation conducted by healthcare providers to better understand the nature and impact of Nutcracker syndrome on an individual basis. Consulting with healthcare professionals can provide personalized guidance on managing symptoms and potential positional variations experienced due to Nutcracker syndrome.
How serious is nutcracker syndrome?
Nutcracker syndrome, while relatively rare, can vary widely in its severity and impact on an individual’s health. In some cases, it might be asymptomatic or cause mild discomfort, while in others, it can lead to more significant symptoms and complications. The seriousness of Nutcracker syndrome depends on several factors:
Severity of Symptoms:
– Mild Cases: Some individuals might have Nutcracker syndrome without experiencing significant symptoms or complications. In these cases, the condition might be discovered incidentally during imaging studies performed for other reasons.
– Moderate to Severe Symptoms: Others might experience noticeable symptoms such as flank pain, hematuria, varicoceles (in males), proteinuria, or abdominal discomfort, which can impact daily life and require medical attention.
Potential Complications:
– Chronic Venous Hypertension: Prolonged venous congestion due to Nutcracker syndrome can lead to increased pressure in the affected vessels, potentially resulting in complications such as renal venous hypertension itself, renal impairment, or changes in the affected kidney.
– Secondary Effects: In more severe or chronic cases, Nutcracker syndrome might contribute to complications that indirectly affect other systems, such as the cardiovascular system or overall venous circulation.
– Varied Impact on Quality of Life: Nutcracker syndrome’s impact on quality of life can vary among individuals. Some might experience minimal disruption, while others might face considerable discomfort or limitations in daily activities due to symptoms.
Nutcracker syndrome’s seriousness varies widely among individuals, ranging from asymptomatic cases to those with significant symptoms and potential complications. Regular evaluation and appropriate management by healthcare professionals are crucial in assessing the condition’s impact, addressing symptoms, and preventing or managing complications associated with Nutcracker syndrome. Early diagnosis and tailored treatment plans can significantly improve the outlook and quality of life for individuals affected by this condition.
Conservative management
Conservative management of Nutcracker syndrome involves non-invasive or minimally invasive approaches aimed at alleviating symptoms and improving the individual’s quality of life without surgical intervention. Here are some key aspects of conservative management:
1. Symptom Management:
Pain Relief:
– Pain Medications: Over-the-counter pain relievers or prescribed medications may help manage discomfort associated with Nutcracker syndrome.
Lifestyle Modifications:
– Activity Adjustment: Avoiding activities that exacerbate symptoms, such as heavy lifting or strenuous exercises, can help reduce discomfort.
2. Supportive Measures:
Compression Stockings:
– Wearing Compression Garments: Compression stockings or garments can assist in managing symptoms related to varicoceles (enlarged veins), reducing discomfort.
3. Regular Monitoring:
Follow-up:
– Regular Check-ups: Scheduled follow-up appointments with healthcare providers for monitoring symptoms and evaluating any changes in the condition are essential.
4. Nutritional and Hydration Considerations:
Dietary Recommendations:
– Balanced Diet: Encouraging a balanced diet to maintain overall health and possibly support vascular health.
Hydration:
– Adequate Hydration: Ensuring proper hydration might have a positive impact on overall vascular function.
5. Observation and Continued Assessment:
Monitoring Symptoms:
– Observation Period: In some cases, healthcare providers may opt for a period of observation to assess whether symptoms stabilize or worsen before considering more invasive treatments.
6. Patient Education and Support:
Information and Resources:
– Educational Resources: Providing information about the condition and its management, as well as support resources or groups, can be beneficial for individuals coping with Nutcracker syndrome.
Limitations of Conservative Management:
– Conservative management might not resolve the underlying compression causing Nutcracker syndrome.
– It aims primarily at symptom relief rather than addressing the anatomical cause directly.
– Effectiveness can vary among individuals, and some may not find sufficient relief through conservative measures alone.
Final Consideration:
While conservative management approaches can offer relief and improve the quality of life for individuals with Nutcracker syndrome, the effectiveness of these measures might vary. In cases where symptoms persist or significantly impact daily life, further interventions like minimally invasive procedures or surgery might be considered after thorough evaluation by healthcare professionals.
Treatment options for Nutcracker Syndrome
The treatment approach for Nutcracker Syndrome depends on the severity of the symptoms and the impact on the individual’s quality of life. In some cases, conservative management may be recommended, which involves lifestyle modifications and symptom management strategies. This may include avoiding triggers that worsen symptoms, such as prolonged standing or physical exertion, and using pain medications as needed.
In more severe cases, medical intervention may be necessary. This can include procedures such vascular surgery such as renal vein stenting, which involves placing a stent in the most compressed vein area to improve blood flow. Other surgical options, such as renal autotransplantation or gonadal vein embolization, may also be considered in certain situations.
Lifestyle changes to manage Nutcracker Syndrome
Making certain lifestyle changes can help manage the symptoms of Nutcracker Syndrome and improve overall well-being. This may include maintaining a healthy diet and weight, engaging in regular exercise, and practicing stress management techniques. It is also important to stay hydrated and avoid activities that may exacerbate symptoms, such as heavy lifting or prolonged sitting or standing.
Conclusion
Nutcracker Syndrome poses significant challenges for patients and their loved ones, impacting their physical, emotional, and mental well-being. By understanding the causes, symptoms, and available treatment options, individuals affected by Nutcracker Syndrome can make informed decisions and seek appropriate healthcare and support. Additionally, emotional support, resources, and awareness initiatives can contribute to enhancing the overall well-being of those living with this rare vascular disorder. Together, we can strive to bring hope, understanding, and improved quality of life to Nutcracker Syndrome patients and their loved ones.