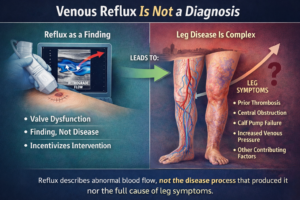
Venous hypertension is a condition characterized by increased blood pressure within the venous system, which is the network of veins responsible for returning deoxygenated blood back to the heart. This condition often results from venous insufficiency, where the veins have trouble sending blood from the limbs back to the heart, often due to weakened or damaged valves that prevent blood from flowing properly.
Understanding venous hypertension is crucial for overall vascular health because it can lead to serious complications if left untreated, such as varicose veins, leg swelling, pain, and even more severe conditions like leg ulcers or deep vein thrombosis.
Recognizing and managing venous hypertension is essential in preventing its progression and maintaining healthy circulation throughout the body, highlighting the importance of vascular health in overall well-being.
What is Venous Hypertension?
– Definition of venous hypertension
Venous hypertension is a medical condition defined by abnormally high blood pressure within the venous system, the network of veins responsible for returning blood to the heart after it has circulated throughout the body.
Unlike arterial hypertension, which occurs in the arteries carrying oxygenated blood from the heart to the body, venous hypertension involves the veins, particularly those in the lower limbs, where blood is supposed to return to the heart against gravity.
This condition is often the result of venous insufficiency, where the venous valves that prevent the backflow of blood are weakened or damaged, leading to blood pooling in the veins.
This pooling increases venous pressure and can cause a range of symptoms and complications, from swelling and discomfort in the affected limbs to more severe outcomes like skin changes, varicose veins, and ulcers, making it a significant concern for vascular health.
– How it differs from arterial hypertension?
Venous hypertension and arterial hypertension represent two distinct conditions within the circulatory system, differentiated primarily by their location and underlying mechanisms.
Arterial hypertension, commonly known as high blood pressure, occurs when the force of the blood against the arterial walls is consistently too high as the heart pumps blood out to the body. This can lead to arterial damage, increased risk of heart disease, stroke, and other cardiovascular issues.
On the other hand, venous hypertension occurs in the venous system, where the pressure within the veins becomes elevated due to the inability of blood to properly return to the heart, often because of valve dysfunction or obstruction.
While arterial hypertension is related to the systemic pressure exerted by blood as it circulates throughout the body, venous hypertension is associated with localized pressure increases, typically in the lower extremities, leading to complications such as swelling, varicose veins, and skin ulcers.
Thus, the key differences lie in their causes, affected areas of the circulatory system, and the nature of health risks they pose.
– Overview of the venous system in the body
The venous system is an extensive network of veins that serves as a critical component of the circulatory system, responsible for returning deoxygenated blood back to the heart from various parts of the body.
This system works in tandem with the arterial system, which delivers oxygen-rich blood from the heart to tissues throughout the body. Veins are equipped with one-way valves that prevent the backflow of blood, facilitating its upward movement against gravity, especially in the lower limbs.
The venous system is categorized into two main types: the deep veins, which are located within muscle tissue and carry the majority of the blood back to the heart, and the superficial veins, which are closer to the skin and less significant in blood transport.
Additionally, the venous system includes the venous sinuses, which are large channels in the brain that collect blood for return to the heart, and the portal vein system, which transports blood from the gastrointestinal tract and spleen to the liver.
Proper functioning of the venous system is vital for maintaining blood volume and pressure balance within the circulatory system, highlighting its importance in overall cardiovascular health.
Causes and Risk Factors
– Causes of venous hypertension
Venous hypertension arises from a multitude of factors that impair the venous system’s ability to efficiently return blood to the heart, leading to increased pressure within the veins. The primary causes include:
1. Venous Insufficiency: This is the most common cause of venous hypertension. It occurs when the valves in the leg veins themselves, which are meant to prevent the backflow of blood, become weakened or damaged. This valve failure allows blood to pool in the veins, particularly in the lower legs, due to gravity, causing increased pressure.
2. Deep Vein Thrombosis (DVT): DVT is the formation of a blood clot in a deep vein, usually in the legs. The clot can obstruct the flow of blood, leading to increased pressure upstream of the obstruction. This not only causes venous hypertension but also poses a risk for pulmonary embolism if the clot dislodges and travels to the lungs.
3. Obesity: Excessive body weight increases the pressure on the veins in the legs and pelvis, contributing to the development of venous hypertension. The additional weight can strain and damage the venous valves, leading to insufficiency.
4. Pregnancy: During pregnancy, the expanding uterus exerts more pressure on the veins in the pelvis and legs. Combined with hormonal changes that can dilate the veins, this can lead to venous hypertension. While temporary for many, it can become a persistent issue for some women post-pregnancy.
5. Prolonged Standing or Sitting: Occupations or lifestyles that involve long periods of standing or sitting can increase the risk of venous hypertension. These positions hinder the normal blood flow and can lead to increased pressure in the veins over time.
6. Age: Aging can lead to wear and tear on the venous valves, reducing their efficiency and increasing the risk of venous hypertension. The natural loss of tissue elasticity with age can also affect the veins’ ability to pump blood effectively.
7. Genetic Factors: There is a hereditary component to venous insufficiency and, by extension, to develop chronic venous insufficiency and hypertension. A family history of vein problems can increase an individual’s risk.
8. Previous Venous Surgery or Trauma: Surgery on the veins or physical trauma can damage the valves or the vein walls, leading to venous hypertension.
These causes highlight the complexity of venous hypertension and underscore the importance of addressing risk factors where possible, through lifestyle changes, medical treatment, or both, to mitigate the condition’s development and progression.
– Risk factors including lifestyle and genetic predispositions
The risk factors for developing venous hypertension are multifaceted, encompassing both lifestyle choices and genetic predispositions. Understanding these risk factors is crucial for prevention and management of the condition.
Lifestyle Factors
1. Prolonged Standing or Sitting: Occupations that require long periods of standing or sitting without movement can significantly increase the risk of venous hypertension. The lack of muscle contraction in the legs impairs the venous return to the heart, leading to increased venous pressure.
2. Obesity: Excess body weight exerts additional pressure on the veins in the legs and abdomen, compromising venous return and contributing to valve dysfunction. The increased pressure can lead to the development of venous hypertension over time.
3. Physical Inactivity: A sedentary lifestyle contributes to poor circulation and can weaken the leg muscles that assist with pumping blood back to the heart, increasing the risk of venous insufficiency and hypertension.
4. Smoking: Smoking affects blood circulation and can damage the structure of blood vessels, increasing the risk of various venous disorders, including venous hypertension.
5. Diet: A diet high in sodium can lead to water retention, which can increase the volume of blood within the veins, thereby increasing venous pressure.
Genetic Predispositions
1. Family History: Individuals with a family history of venous insufficiency, varicose veins, or venous ulcers are at a higher risk for developing venous hypertension. Genetic factors can influence the strength and functionality of the venous valves and the elasticity of the vein walls.
2. Age: The risk of venous hypertension increases with age, partly due to the natural degradation of venous valves and loss of elasticity in the vein walls, which are conditions that can be exacerbated by genetic predispositions to tissue weakness.
3. Gender: Women are more likely to develop venous disorders, including venous hypertension, possibly due to hormonal influences that affect vein elasticity and valve functionality. This risk is further increased by pregnancy, especially multiple pregnancies, which can stress the venous system.
4. Hormonal Factors: Hormonal changes, such as those occurring during pregnancy, menopause, or as a result of hormonal therapy or contraception, can affect the venous system. Genetic sensitivity to these changes can increase the risk of developing venous hypertension.
Interaction of Factors
The interplay between lifestyle and genetic factors significantly influences the risk of developing venous hypertension. For instance, an individual with a genetic predisposition to weak venous valves may be more likely to develop venous hypertension if they also have a lifestyle that includes prolonged periods of standing, obesity, or smoking.
Conversely, individuals with a strong genetic predisposition might still mitigate their risk through proactive lifestyle choices, such as maintaining a healthy weight, exercising regularly, and avoiding long periods of inactivity.
Understanding these risk factors allows for targeted interventions, including lifestyle modifications and medical treatments, to prevent or manage venous hypertension effectively.
Symptoms and Diagnosis
– Description of common symptoms associated with venous hypertension.
Venous hypertension manifests through a variety of symptoms, reflecting the increased pressure in the venous system and its impact on circulation. Common symptoms associated with venous hypertension include:
1. Leg Swelling (Edema): One of the most noticeable symptoms, swelling in the legs and ankles occurs due to the accumulation of fluid in the tissues, a direct result of increased venous pressure.
2. Varicose Veins: These are enlarged, swollen veins that appear twisted and bulging under the skin, commonly seen in the legs. Varicose veins develop when the increased pressure in the veins causes the valves to fail, allowing blood from healthy vein to pool.
3. Leg Heaviness and Fatigue: Individuals with venous hypertension often report a sensation of heaviness or tiredness in their legs, which can worsen after prolonged standing or sitting and typically improves with leg elevation.
4. Pain or Aching: The increased pressure and swelling can cause discomfort, pain, or a throbbing sensation in the legs, which may also worsen by the end of the day or after long periods of inactivity.
5. Itching and Tingling: The accumulation of blood and increased pressure can irritate the skin, leading to itching or tingling sensations around the affected veins.
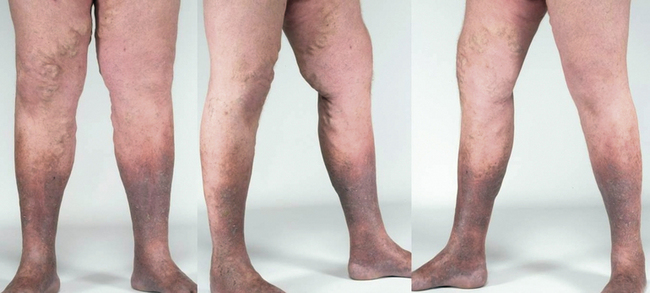
6. Skin Changes: Over time, chronic venous hypertension also can lead to skin changes such as discoloration, thickening, and the development of eczema-like rashes. These changes are due to poor oxygenation and nutrition of the skin caused by impaired venous return.
7. Venous Ulcers: In advanced cases, prolonged venous hypertension can result in venous ulcers, which are open sores that develop on the skin and are slow to heal. These ulcers are typically found on the inner aspect of the leg, just above the ankle, where venous pressure is greatest.
8. Bleeding: Minor injuries to the area can lead to more significant bleeding than usual due to the increased pressure in the veins.
– How venous hypertension is diagnosed, including medical tests and evaluations?
Diagnosing venous hypertension involves a combination of clinical evaluation and diagnostic tests to assess the function of the venous system and identify the underlying causes of increased venous pressure. The diagnostic process typically includes:
Clinical Evaluation
1. Medical History: A detailed medical history helps identify risk factors such as family history of venous disease, previous venous thrombosis, lifestyle factors, and symptoms that suggest deep venous thrombosis or hypertension.
2. Physical Examination: The doctor examines the legs for signs of venous disease, including swelling, varicose veins, skin changes, and ulcers. The assessment may also involve checking for signs of fluid accumulation or changes in skin temperature and color.
Diagnostic Tests
Several tests can further evaluate the structure and function of the veins, confirming the diagnosis and helping to plan treatment.
1. Doppler Ultrasound: This is the most common test for diagnosing venous hypertension. It uses sound waves to visualize blood flow and can identify any abnormalities in the venous system, such as valve dysfunction or evidence of deep vein thrombosis (DVT). Doppler ultrasound can assess both the superficial and deep venous systems.
2. Duplex Ultrasound: A more detailed form of Doppler ultrasound, duplex ultrasound combines traditional ultrasound to visualize the veins with Doppler flow studies to assess blood movement. It provides images of the veins and shows how blood is flowing through them, helping to pinpoint areas of valve failure or obstruction.
3. Venography: Although less commonly used today due to the non-invasive nature of ultrasound, venography involves injecting a contrast dye into the veins and taking X-rays. This procedure can provide detailed images of the veins, revealing blockages or valve problems not detected by ultrasound.
4. Ambulatory Venous Pressure Testing: This test measures the pressure in the veins of the lower legs during exercise and rest. It involves inserting a needle connected to a pressure monitor into a vein in the foot and is used to quantify venous insufficiency.
5. Photoplethysmography (PPG): A PPG test measures changes in blood volume in the skin, providing information about the efficiency of blood return to the heart. It’s a non-invasive test that uses a special sensor placed on the skin.
Additional Evaluations
Depending on the findings from the initial tests, additional assessments might be necessary to rule out other conditions or to evaluate the extent of complications associated with venous hypertension, such as:
– CT or MRI scans: These imaging tests can provide detailed images of the venous system and surrounding structures, useful in complex cases or when planning surgical interventions.
– Blood tests: While not used to diagnose venous hypertension directly, blood tests can identify clotting disorders or other underlying conditions that might contribute to venous problems.
A comprehensive diagnostic approach ensures accurate identification of venous hypertension and its causes, allowing for effective treatment planning tailored to the individual’s condition.
Complications
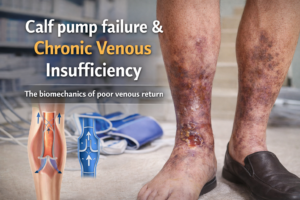
If venous hypertension remains untreated, it can lead to a cascade of complications that significantly impact quality of life and overall health. Two of the most concerning potential outcomes are venous ulcers and chronic venous insufficiency, each representing advanced stages of chronic venous disease with their own set of challenges and implications.
Chronic Venous Insufficiency (CVI)
Chronic venous insufficiency occurs when the venous system fails to effectively return blood from the limbs back to the heart, leading to prolonged venous hypertension. This condition is often a progression from untreated venous hypertension and is characterized by:
– Persistent Swelling: Due to the accumulation of fluid in the tissues, leading to chronic edema.
– Skin Changes: Including hyperpigmentation, where the skin turns a brownish color due to the breakdown of red blood cells and the deposition of hemosiderin; eczema-like changes; and lipodermatosclerosis, a hardening of the skin and fat beneath the skin.
– Varicose Veins: Worsening of existing varicose veins or development of new ones.
CVI is not only uncomfortable but can also significantly impair mobility and daily activities, leading to a decreased quality of life.
Venous Ulcers
Venous ulcers are one of the most severe complications of venous hypertension and CVI. They are open sores that typically develop on the inner aspect of the leg, just above the ankle, where venous pressure from damaged veins is highest. Venous ulcers are often:
– Difficult to Heal: The impaired circulation affects the delivery of oxygen and nutrients necessary for wound healing.
– Recurrent: Without addressing the underlying venous hypertension, ulcers can heal and then reopen.
– Painful: The ulcers can be very painful, impacting an individual’s ability to perform daily activities.
The development of venous ulcers signifies a significant progression in venous disease, requiring comprehensive treatment to manage the wound and address the venous insufficiency.
Other Complications
In addition to CVI and venous ulcers, untreated venous hypertension can lead to several other complications:
– Superficial Thrombophlebitis: Inflammation of a superficial vein that can cause pain, redness, and swelling along the course of the vein.
– Deep Vein Thrombosis (DVT): Although DVT is more often a cause of venous hypertension, ongoing venous hypertension can increase the risk of further clot formation.
– Cellulitis: The skin changes and ulcers associated with venous hypertension can increase the risk of bacterial skin infections, such as cellulitis.
The progression from venous hypertension to chronic venous insufficiency and venous ulcers highlights the importance of early detection and treatment of venous disorders.
Effective management of venous hypertension can prevent or slow the progression to more severe complications, improving outcomes and quality of life for those affected.
Treatment strategies can include lifestyle modifications, compression therapy, medications, and, in some cases, surgical interventions to correct the underlying venous abnormalities.
Treatment and Management
– Overview of treatment options ranging from lifestyle changes to medical interventions.
Treating venous hypertension involves a comprehensive approach that aims to alleviate symptoms, prevent progression of the disease, and manage any complications. Treatment options range from conservative lifestyle changes to more invasive medical interventions. The choice of treatment depends on the severity of the condition, the presence of complications, and the individual’s overall health status.
Lifestyle Changes and Self-care
1. Elevation of the Legs: Regularly elevating the legs above heart level helps reduce venous pressure and swelling.
2. Exercise: Regular, moderate exercise, especially walking, improves muscle tone and promotes better venous circulation.
3. Weight Management: Maintaining a healthy weight reduces pressure on the veins and can alleviate symptoms.
4. Compression Stockings: Wearing graduated compression stockings helps squeeze the legs, promoting blood flow back to the heart and reducing swelling and discomfort.
Medications
1. Diuretics: Sometimes used to reduce swelling, although not a standard treatment for venous hypertension as they do not address the underlying venous insufficiency.
2. Anticoagulants: For individuals with deep vein thrombosis, anticoagulant medication can prevent clot progression and reduce the risk of pulmonary embolism.
3. Pentoxifylline or Aspirin: These medications can improve blood flow and might be used in conjunction with other treatments to heal venous ulcers.
Minimally Invasive Procedures
1. Sclerotherapy: Involves injecting a solution into small to medium-sized varicose veins, causing them to scar and close, rerouting blood to healthier veins.
2. Endovenous Thermal Ablation: Uses heat generated by laser or radiofrequency to close off varicose veins.
3. Ultrasound-guided Foam Sclerotherapy: A variation of sclerotherapy that uses a foam solution to treat larger veins.
Surgical Interventions
1. Ligation and Stripping: The surgical removal or tying off of large varicose veins.
2. Phlebectomy: Small incisions are made to remove varicose veins that are close to the surface of the skin.
3. Vein Bypass: In severe cases, especially in the upper thigh, a vein from another part of the body may be transplanted to bypass the damaged vein.
Advanced Treatments for Complications
– Wound Care: For venous ulcers, specialized wound care, including debridement, dressings, and possibly skin grafting, is necessary.
– Compression Therapy: Continues to be a cornerstone for managing the symptoms of chronic venous insufficiency and healing venous ulcers.
Considerations
The choice of treatment is highly individualized, taking into account the specific needs and circumstances of the patient. For many, a combination of treatments may offer the best results. Regular follow-up with a healthcare provider is crucial to monitor the effectiveness of the treatment plan and make adjustments as necessary. Early intervention and a proactive approach can significantly improve outcomes for individuals with venous hypertension.
Conclusion:
Venous hypertension is a complex vascular condition causing elevated pressure in the venous system. It can be caused by various factors such as venous insufficiency, deep vein thrombosis, obesity, prolonged standing, age, genetic predispositions, and lifestyle factors.
Symptoms include leg swelling, varicose veins, pain, itching, skin changes, and in severe cases, venous ulcers. Management strategies include lifestyle modifications, medications, and minimally invasive procedures and surgical interventions.
Early detection and personalized treatment plans are crucial for managing the condition. Regular follow-ups and adjustments to treatment strategies are essential to address the evolving nature of the condition.
Understanding the causes, recognizing symptoms early, and combining lifestyle changes and medical interventions can significantly improve outcomes for individuals with venous hypertension, enhancing their quality of life and vascular health.