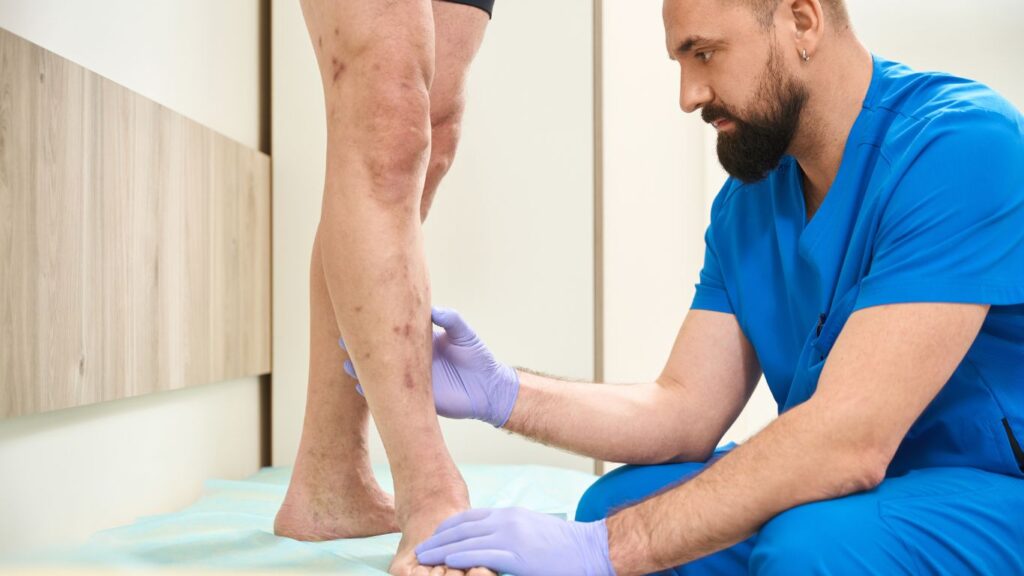
Post-Thrombotic Syndrome
under-recognised cause of long-term leg pain, swelling, skin damage, and venous ulceration after deep vein thrombosis (DVT).
What is post-thrombotic syndrome?
Post-thrombotic syndrome (PTS) develops when a previous DVT damages the deep venous system, leading to chronic venous hypertension. This can result in:
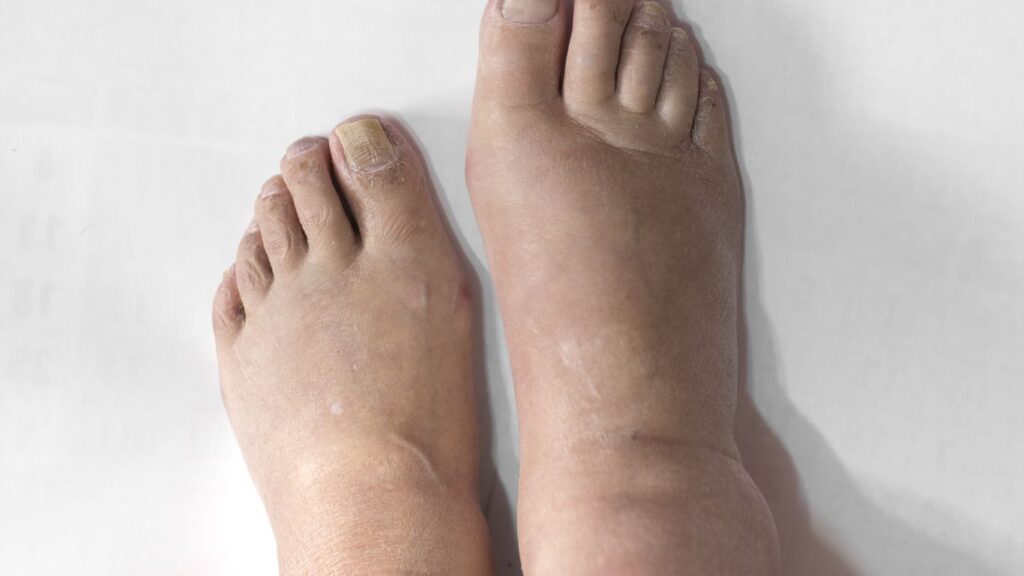
- persistent leg swelling
- heaviness or aching
- skin pigmentation changes
- venous eczema
- lipodermatosclerosis
- recurrent or non-healing ulcers
Symptoms may appear months or even years after the original clot.
Early structured management significantly improves long-term outcomes.
Who should attend this clinic?
You may benefit from assessment if you have:
- previous deep vein thrombosis
- persistent leg swelling after DVT
- skin changes in one leg following thrombosis
- recurrent venous ulceration
- new varicose veins developing after DVT
- heaviness or discomfort not explained by primary venous disease
These symptoms frequently indicate evolving post-thrombotic venous insufficiency.
Our role as your diagnostic gateway
Our clinic provides post-thrombotic syndrome management. We provide structured assessment and referral pathways so patients reach the right specialists efficiently.
Following evaluation:
- A personalised management plan is created
- Compression strategies are optimised
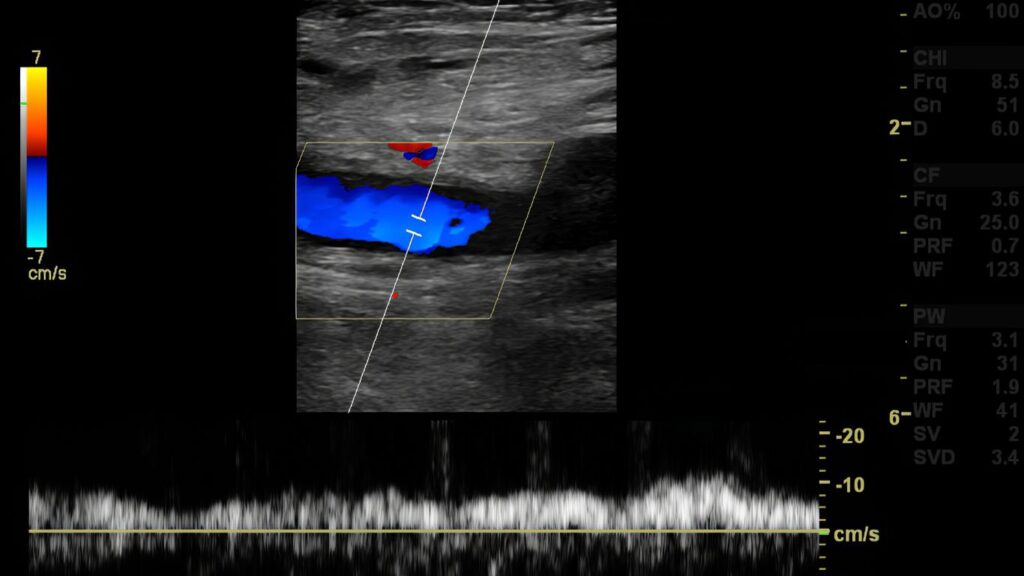
- Reflux patterns are documented and explained
- Ulcer prevention pathways are initiated if required
- Referral for advanced venous intervention is arranged when appropriate
This structured approach supports both symptom control and long-term limb preservation.