Lymphoedema is a chronic condition characterised by the accumulation of lymphatic fluid in the tissues, leading to swelling, discomfort, and impaired functionality.
It occurs when the lymphatic system, responsible for fluid drainage and immune function, becomes compromised or damaged. Lymphoedema can be either primary (congenital or hereditary) or secondary (resulting from an underlying medical condition, injury, or treatment).
This condition often affects the arms, legs, or other body parts, causing persistent swelling that can have a significant impact on a person’s quality of life. Understanding the causes, symptoms, and management options for lymphoedema is crucial in providing appropriate care and support for individuals affected by this condition.
What causes lymphoedema?

Lymphoedema can be caused by various factors that result in damage or obstruction to the lymphatic system or lymph nodes. The primary causes of lymphoedema of the lymphatic drainage or nodes include:
1. Primary Lymphoedema:
Primary lymphoedema refers to a form of lymphoedema that is present at birth or develops later in life due to an inherited or genetic predisposition.
It occurs when there is a congenital abnormality or dysfunction in the lymphatic system, leading to impaired fluid drainage and the accumulation of lymphatic fluid in the affected areas.
Primary lymphoedema can manifest in various ways, ranging from mild swelling to more severe and extensive swelling in the limbs or other parts of the body.
The condition may present at birth or become apparent later in life, often during puberty or adulthood. Understanding the underlying causes and specific characteristics of primary lymphoedema is essential in diagnosing and managing this chronic condition effectively
2. Secondary Lymphoedema:
Secondary lymphoedema is a type of lymphoedema that occurs as a result of damage or obstruction to the lymphatic system. Unlike primary lymphoedema, which is typically caused by inherited factors, secondary lymphoedema is acquired and can develop as a consequence of various underlying conditions or factors.
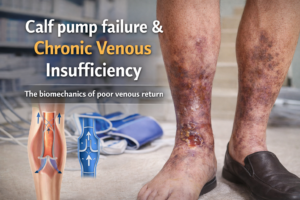
These may include surgery or radiation therapy for cancer treatment, trauma or injury to the lymphatic system, infections, such as cellulitis, or other medical conditions that affect the lymphatic system, such as venous insufficiency.
Secondary lymphoedema occurs and is characterised by swelling and fluid retention in lymph tissue of lymph nodes and vessels in the affected area, which can cause discomfort, limited mobility, and potential complications if left untreated. Early identification and appropriate management of the underlying cause are crucial in minimising the progression and impact of secondary lymphoedema on the affected individuals.
It’s important to note that while primary lymphoedema is often caused by genetic factors, secondary lymphoedema can have multiple triggers and may vary from person to person. Understanding the underlying cause is essential in managing and treating primary and secondary lymphoedema more effectively.

What are the risk factors for developing lymphoedema?
Several risk factors can increase the likelihood of developing lymphoedema. These include:
1. Surgery:
Surgical procedures that involve lymph node removal or damage to the lymphatic system, such as breast cancer surgery or lymph node dissection, or radiation treatment can increase the risk of lymphoedema.
2. Radiation Therapy:
Radiation therapy, often used as a treatment for cancer, can cause scarring of cancer cells and inflammation of the lymphatic vessels, leading to lymphoedema.
3. Cancer:
Certain types of cancer, such as breast cancer, prostate cancer, gynecological cancers, breast cancer and melanoma, are associated with a higher risk of developing lymphoedema.
4. Infections:
Repeated or severe infections that affect lymphatic vessels in any part of the body or lymphatic system, such as cellulitis, can damage the lymphatic and blood vessels, and contribute to the development of lymphoedema.
5. Obesity:
Excess weight can put additional strain on the lymphatic system, impeding its proper function and increasing the risk of lymphoedema.
6. Age:
Lymphoedema can occur at any age, but it is more commonly seen in older individuals as the lymphatic system’s efficiency may decline with age.
7. Genetic Factors:
In some cases, there may be a genetic predisposition to developing lymphoedema, especially in primary lymphoedema cases.
It’s important to note that while these risk factors may increase the likelihood or risk of developing lymphoedema itself, not everyone with these factors will develop the condition. It is essential to be aware of these risks and take appropriate preventive measures, especially for individuals who have undergone lymphatic system-related surgeries or treatments.
What are the symptoms of lymphoedema?

The symptoms of lymphoedema can vary depending on the severity of the condition. Common signs and symptoms of lymphoedema include:
1. Swelling:
Persistent swelling, often in the arms or legs, is the hallmark symptom of lymphoedema. The swelling can range from mild to severe and may be accompanied by a feeling of heaviness or tightness in the affected limb.
2. Increased size:
The affected limb may appear larger or feel full and puffy compared to the unaffected limb. The swelling may worsen over time if bacterial infection is left untreated.
3. Limited range of motion:
As the swelling progresses, it can restrict movement and flexibility in the affected limb, making it difficult to perform everyday tasks or engage in physical activities.
4. Aching or discomfort:
Some individuals with lymphoedema may experience aching, discomfort, or a sensation of heaviness in the affected limb.
5. Skin changes:
The skin over the swollen area may feel tight, firm, or thickened. It may also appear red, warm to the touch, or develop a shiny or hardened texture.
6. Recurrent infections:
Due to impaired lymphatic flow, individuals with lymphoedema may be more prone to developing skin infections, such as cellulitis.
If you notice any persistent swelling or other symptoms suggestive of lymphoedema, it is important to consult with a healthcare professional for a proper diagnosis and management plan. Early intervention and appropriate treatment can help manage symptoms, prevent complications, and improve overall quality of life.
What are the 3 stages of lymphedema?

The staging system for lymphoedema typically includes three stages based on the severity of the condition:
1. Stage 1:
This stage is characterised by mild swelling that subsides when blood pressure readings the affected arm or leg, leg or limb is elevated. The swelling may not be noticeable initially, or it may come and go. The skin texture remains normal, and pitting oedema is not visible swelling is not present.
2. Stage 2:
In this stage, the swelling becomes more persistent and does not fully resolve with elevation. Pitting edema is evident, meaning that when pressure is applied to the swollen area, it leaves a temporary indentation. The skin may start to show changes, such as thickening, fibrosis, or discoloration.
3. Stage 3:
The most advanced stage of lymphoedema, stage 3 involves significant swelling that is constant and often accompanied by hardening of the affected tissue fluid limb. Fibrotic changes occur in the underlying tissues throughout the affected body part, causing a loss of elasticity. Skin changes, such as thickening, hardening (known as fibroadhesions), and discoloration, are pronounced. Recurrent infections, called cellulitis, are also common at this stage.
It’s important to note that the staging of lymphoedema can vary slightly depending on the classification system used and individual patient characteristics. It is best to consult with a healthcare professional specialising in lymphoedema for an accurate diagnosis and appropriate management plan.
How is lymphoedema diagnosed?
Lymphoedema is typically diagnosed through a combination of medical history, physical examination, and diagnostic blood tests done. The diagnostic process may involve the following:
1. Medical history:
The healthcare provider will review your medical history, including any relevant information about previous surgeries, cancer treatments, or other conditions that may increase the risk of lymphoedema.
2. Physical examination:
The healthcare provider will conduct a thorough physical examination, focusing on the affected area(s) and assessing for signs of swelling, skin changes, or other related symptoms. They may also measure and compare the size and circumference of the affected and unaffected limbs.
3. Imaging tests:
Various imaging tests may be used to assess the lymphatic system and determine the extent of lymphoedema. These may include lymphoscintigraphy, which involves injecting a radioactive tracer into the tissues to track the flow of lymphatic fluid, or other imaging techniques such as MRI or ultrasound.
4. Lymphedema Index:
The Lymphedema Index, also known as the Stemmer sign, is a physical examination maneuver where the healthcare provider attempts to pinch the skin at the base of the affected digit or limb. If the skin cannot be lifted or pinched (known as a positive Stemmer sign), it suggests the presence of lymphoedema.
5. Measurement of limb volume:
In some severe cases, volumetric measurements may be performed using specialized equipment to assess the extent of limb swelling and monitor changes over time.
It is important to consult with a healthcare professional experienced in diagnosing and managing lymphoedema for a comprehensive evaluation and accurate diagnosis. They will consider your medical history, perform a thorough examination, and order any necessary tests to confirm the presence of lymphoedema and guide appropriate treatment.
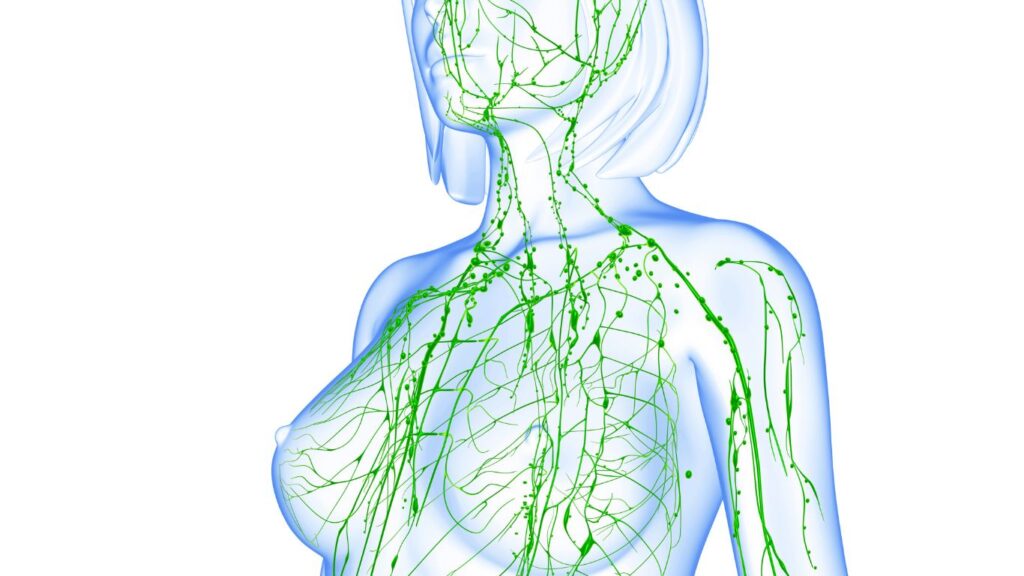
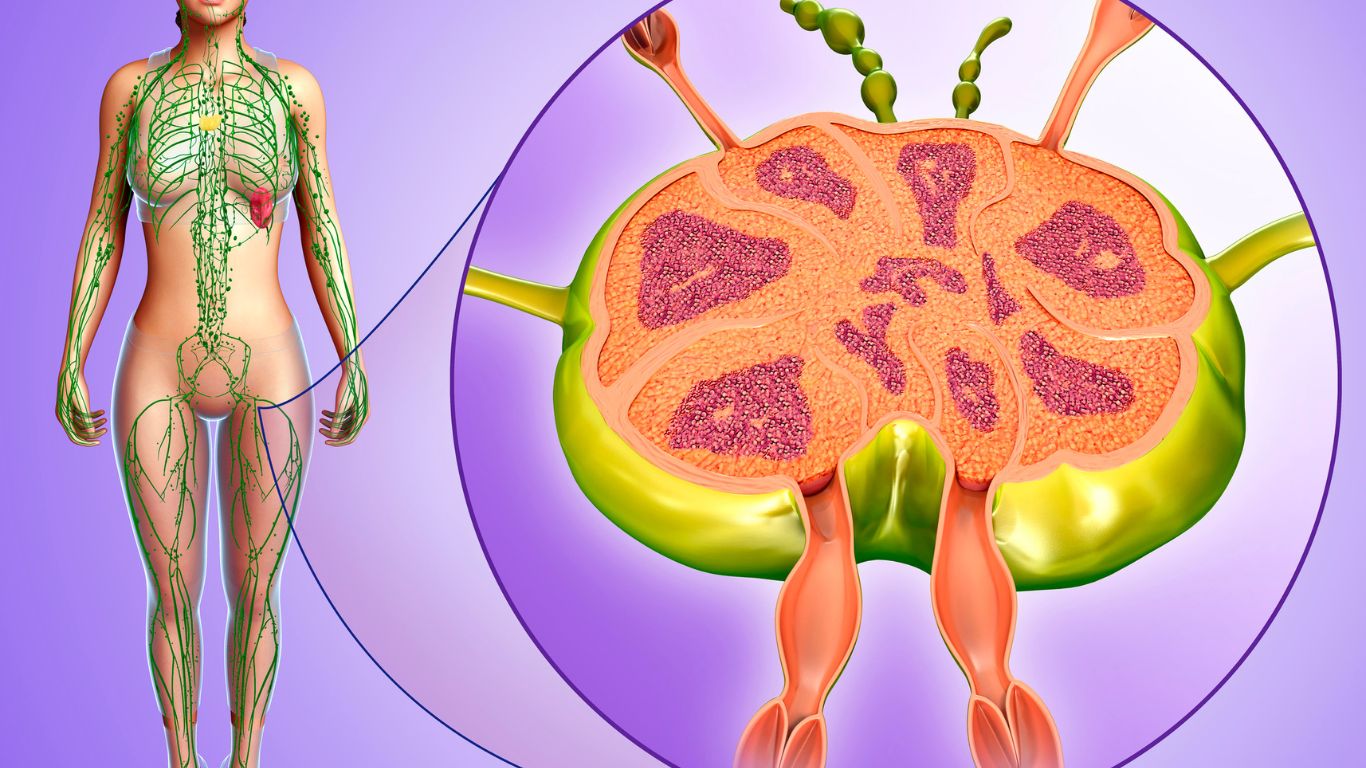
What is the Anatomy of Lymphatic system?
The lymphatic system is a vital network of vessels, tissues, and organs that plays a crucial role in maintaining the body’s fluid balance, immune function, and waste removal. It works in conjunction with the circulatory system to ensure proper circulation and drainage of lymph, a clear fluid containing white blood cells.
The primary components of the lymphatic system include lymphatic vessels, lymph nodes, lymphoid organs (such as the spleen and thymus), and lymphatic tissue scattered throughout the body. Lymphatic vessels, similar to blood vessels, form an extensive network that transports lymph fluid throughout the body. These vessels have one-way valves that allow lymph to flow in only one direction, preventing backflow.
Lymph nodes are small, bean-shaped structures located along the lymphatic vessels. They act as filters, trapping and removing foreign particles, such as bacteria, viruses, and abnormal cells, from the lymph fluid. Lymphoid organs, such as the spleen and thymus, produce and store lymphocytes, a type of white blood cell that plays a key role in the immune response.
The lymphatic system acts as a drainage system, collecting excess fluid, waste products, and cellular debris from the body’s tissues. It helps maintain fluid balance by returning the collected fluid, now called lymph, back into the bloodstream. Additionally, the lymphatic system helps defend the body against infections by transporting immune cells and antibodies to the site of infection.
In summary, the lymphatic system is a complex network that performs essential functions in maintaining fluid balance, immune function, and waste removal. Understanding its anatomy and role is crucial for comprehending how this intricate system contributes to overall health and well-being.
Lymphoedema progression and associated skin changes
Lymphoedema, a condition characterized by swelling and fluid retention, can lead to various skin changes. These skin changes occur due to the accumulation of protein-rich lymph fluid, in the affected body area and the impaired lymphatic system’s inability to further remove excess lymph fluid flow, and waste products. Here are some common skin changes associated with lymphoedema
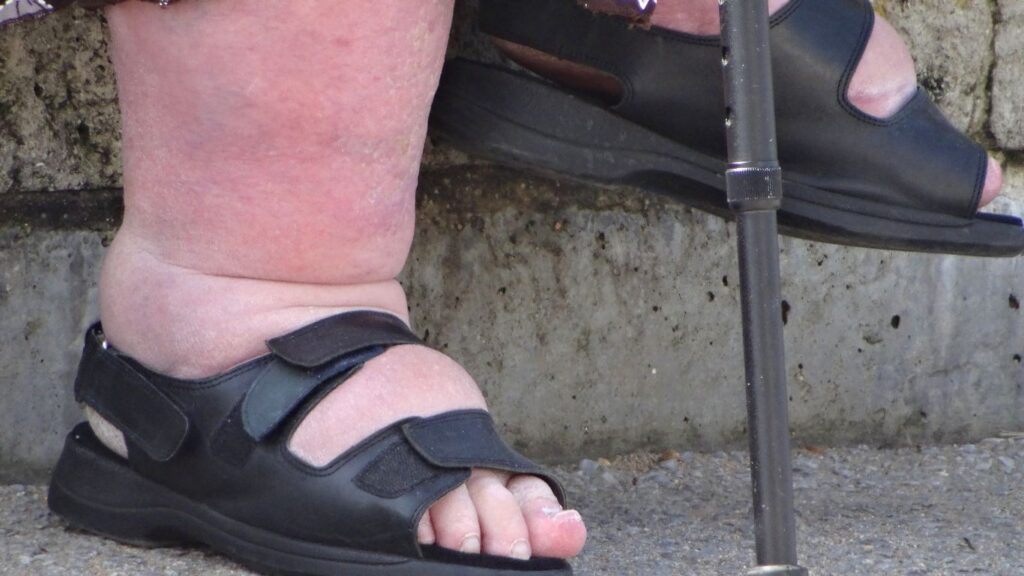
1. Thickening of the Skin:
Over time, the skin affected by lymphoedema may become thickened, firm, and hardened. This occurs due to the deposition of fibrotic tissue caused by chronic fluid buildup in the lymphatic vessels of body tissues and vessels surrounding tissues.
2. Skin Discoloration:
Lymphoedema can cause changes in skin color. The affected area may appear red, bluish, or brownish. This discoloration is often a result of decreased oxygen supply, tissue damage, and the presence of stagnant fluid or swollen tissue.
3. Dryness and Flaking:
The skin in the affected area may become dry, scaly, and prone to flaking. The accumulation of excess fluid also can disrupt the skin’s natural moisture balance, leading to dryness and an increased risk of developing from and susceptibility to skin problems.
4. Infections:
Lymphoedema can make the skin and the part of the body affected much more vulnerable to infections. Bacterial, fungal, or cellulitis infections may occur due to the compromised integrity of the skin barrier and the impaired immune system response in the affected area.
5. Wounds and Ulcers:
In advanced stages of lymphoedema, chronic swelling and poor tissue health can lead to the development of wounds or ulcers. These open sores can be slow to heal and require specialized wound care management.
6. Increased Sensitivity:
The skin affected by lymphoedema may become more sensitive and prone to irritation. It can feel tender, itchy, or painful, further impacting the individual’s comfort and quality of life.
Managing lymphoedema-associated skin changes involves proper skincare, moisturization, and preventive measures to minimize the risk of infection and skin breakdown.
Regular assessment by a healthcare professional experienced in lymphoedema management is crucial to identify and address any skin-related issues promptly. They can recommend appropriate skincare routines, provide guidance on wound care, and offer treatment options to alleviate symptoms and improve skin health.

Treatment and management
The treatment and management of lymphoedema aim to control and prevent infection, reduce swelling, improve symptoms, and prevent complications. While there is no cure for lymphoedema, a combination of strategies can effectively manage the condition. Here are some common approaches to treating lymphoedema:
1. Manual Lymphatic Drainage (MLD):
This is a specialised massage technique performed to remove the lymphatic drainage and remove lymph nodes, by a trained therapist to stimulate lymphatic flow carry lymph fluid and reduce swelling.
2. Compression Therapy:
Wearing compression garments, such as compression garments as, compression bandages, or other compression garments or stockings, helps to apply pressure on the affected limb and promote the movement of lymph fluid.
3. Exercise:
Engaging in regular low-impact exercises, such as walking, swimming, or cycling, can help improve lymphatic flow, muscle strength, and overall lymphatic circulation itself.
4. Skin Care:
Proper skin care is essential in managing lymphoedema. Keeping the skin clean, moisturised, and protected from injury or infection is crucial to prevent skin infection too. Avoiding extremes of temperature and using gentle skincare products are also recommended.
5. Weight Management:
Maintaining a healthy weight can help reduce the strain on the lymphatic system and improve overall lymphoedema management.
6. Dietary Modifications:
Following a balanced, healthy diet with, low in salt and processed foods, can help minimise fluid retention and support the lymphatic system function.
7. Self-Care and Education:
Learning self-care techniques, such as self-massage and exercises, can empower individuals to manage their lymphoedema independently. Education about the condition and its management is important for long-term success.
8. Supportive Measures:
Emotional support and counselling can be beneficial in coping with the challenges of living with lymphoedema. Support groups and online communities can provide valuable resources and a sense of community.
It is essential to consult with a healthcare professional experienced in managing lymphoedema to develop an individualised treatment plan. They can provide guidance, monitor progress, and make necessary adjustments to optimise management and improve quality of life.