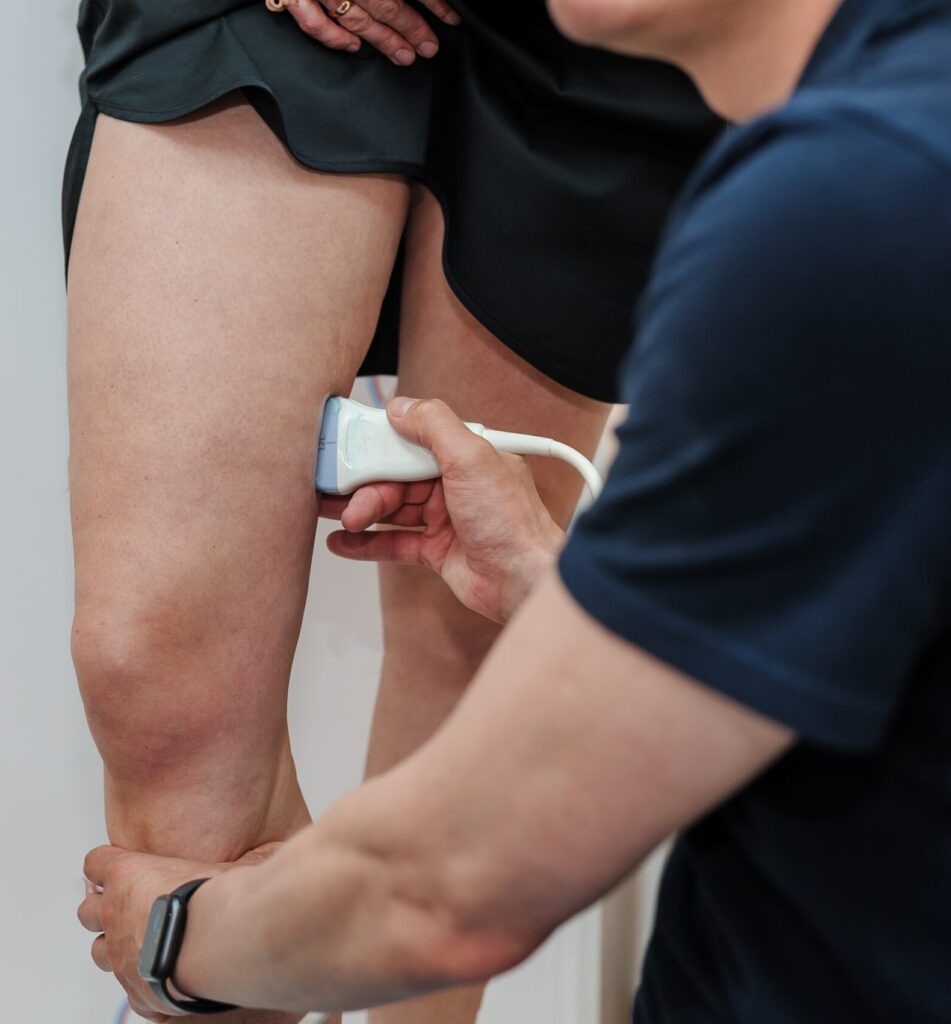
Complex Vein Compression
&
outflow disorders
We specialise in diagnosing and managing pelvic congestion syndrome, May-Thurner syndrome, nutcracker syndrome, and venous malformations.
Vein Compression Syndromes
We assess and manage venous outflow problems caused by compression of major veins.
These conditions are often underdiagnosed and can cause pain, swelling, heaviness, pelvic discomfort, or unexplained symptoms.
Our focus:
- identifying venous obstruction
- assessing flow and anatomy
- correlating symptoms with imaging
- providing treatment or referral pathways for advanced interventions
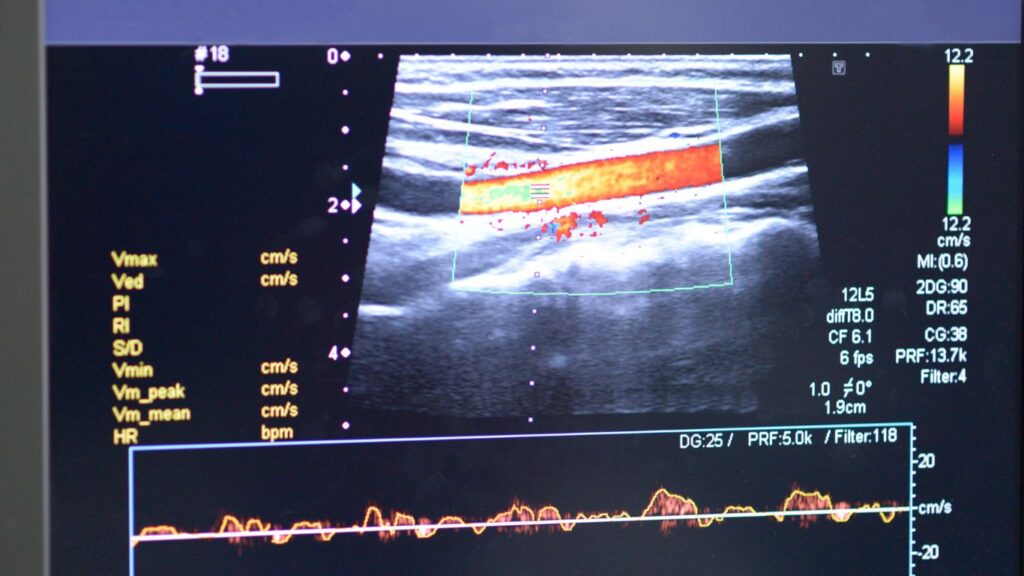
Example of complex vein conditions
Pelvic Congestion Syndrome (PCS)
Pelvic congestion syndrome happens when the veins in the pelvis become stretched and enlarged, which makes it difficult for blood to flow properly. PCS is often overlooked or mistaken for other causes of pelvic pain, but with the right diagnosis, there are effective treatments that can bring lasting relief.
May-Thurner Syndrome
May-Thurner syndrome occurs when the right iliac artery presses down on the left iliac vein, limiting blood flow from the left leg back toward the heart. This “traffic jam” in the vein can lead to symptoms such as swelling, aching, or cramping in the leg — and in some cases, it increases the risk of blood clots.
Nutcracker syndrome
Nutcracker syndrome develops when the left renal vein is squeezed, often between the abdominal aorta and another nearby artery. This compression can disrupt blood flow from the kidney, leading to symptoms such as flank pain, pelvic discomfort, or even blood in the urine.
Venous malformations
Venous malformations are clusters of abnormal veins that are either present at birth or appearing later in life. These veins don’t function like normal blood vessels and can cause swelling, tenderness, or visible skin discoloration.
Vein Problems in Connective Tissue & Hypermobility Conditions
People living with conditions such as joint hypermobility, hypermobility spectrum disorders, or Ehlers–Danlos–type syndromes often experience:
fragile veins
easy bruising
venous pooling
spider and varicose veins
leg swelling and heaviness
chronic discomfort or itch
delayed healing
We provide gentle, tailored vein assessment and treatment for patients with connective-tissue–related venous issues, using techniques appropriate for sensitive or fragile vein structures.
We work collaboratively and transparently, focusing on the vein-related aspects of these conditions.
How we care for you
Step 1: Listen & Learn
Your care begins with your story. We take time to understand your symptoms — when they started, how they’ve changed, and how they affect your daily life. This first step ensures that we see the full picture, not just the medical facts.
Step 2: Diagnose with Precision
Next, we use advanced diagnostic tools such as ultrasound, CT scans, or venography to evaluate your veins in detail. These imaging studies allow us to identify the exact cause of your condition, whether it’s a compressed vein, a malformation, or faulty circulation.
Our goal is always to combine the right therapies for your unique situation — helping you find relief, protect your long-term vein health, and restore confidence in your daily life.
Step 3: Tailored Treatment Plan
Once we have a clear diagnosis, we design a treatment plan that is carefully tailored to your specific needs. Because complex venous conditions can affect more than one system in the body, your care may involve a multidisciplinary team. This could include a vascular surgeon, an interventional radiologist, a plastic surgeon, or other specialists working together to ensure every aspect of your condition is addressed. Treatments may range from compression therapy and lifestyle guidance to minimally invasive procedures such as embolization or stenting. By combining expertise across specialties, we aim to not only relieve your symptoms but also improve circulation, protect long-term vein health, and restore confidence in your everyday life.