Venous leg ulcers can be a debilitating condition for those who suffer from it. These open wounds, usually found on hardened skin of the lower legs, can be painful and difficult to heal. However, there is hope on the horizon as innovative treatments are being developed to help patients on their road to recovery.
In this article, we will explore some of the latest advancements in the field of treatment of venous ulcer. From cutting-edge technologies to novel therapeutic approaches, we will delve into the potential solutions that could revolutionise the management of this chronic condition.
This article aims to provide a comprehensive understanding of the innovative treatments available, giving patients and healthcare professionals valuable insights into the future of venous leg ulcer care.
It’s time to take a step towards recovery. Join us as we discover how these groundbreaking treatments are offering new hope and improving the lives of those affected by venous leg ulcers.
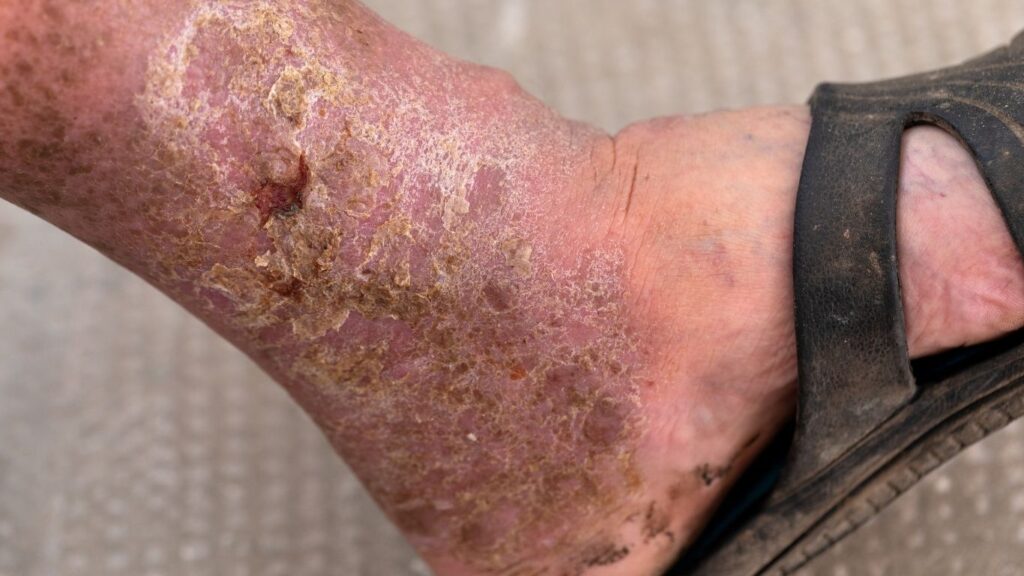
Understanding the causes and symptoms of venous leg ulcers
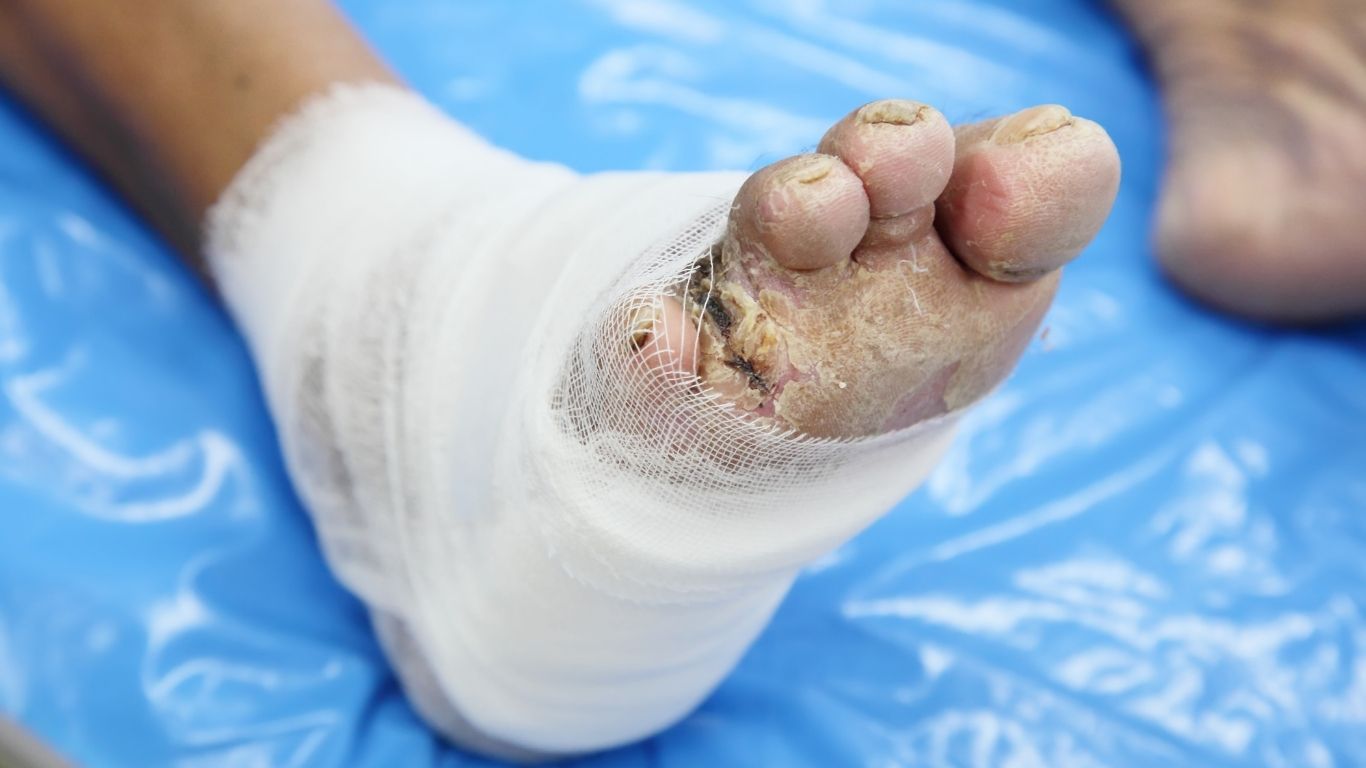
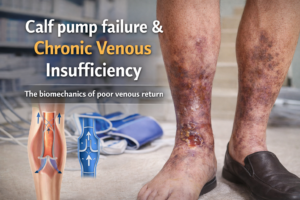
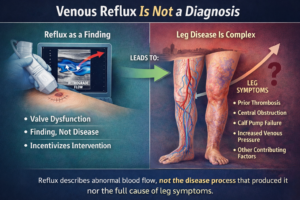
Chronic venous leg ulcers are a result of venous insufficiency, a condition where the veins in the legs are unable to pump blood back to the heart efficiently. This leads to a buildup of pressure in the leg veins, causing damage to the skin and the underlying tissues. The damaged skin then breaks down, leading to the formation of a venous leg ulcer.
The symptoms of venous ulcers include pain, swelling, and the presence of an open wound on the legs. The wound may also be surrounded by discoloured skin, and in severe cases, the surrounding skin of affected leg may become hardened and thickened.
Conventional treatment of venous leg ulcer
Conventional treatments for venous leg ulcers include compression therapy, the use of advanced wound dressings, and the application of topical ointments. Compression therapy involves the use of compression stockings or bandages to improve blood flow and reduce leg swelling below.
Advanced wound dressings such as hydrocolloid dressings and foam dressings are used to promote healing while protecting the wound from infection. Topical ointments such as zinc oxide and silver sulfadiazine are used treat venous leg ulcers to reduce inflammation and prevent infection.
While these treatments are effective, they have their limitations. Compression therapy can be uncomfortable and difficult to wear for extended periods. Advanced wound dressings can be expensive, and the selection of the right dressing can be challenging. Topical ointments can also cause adverse reactions in some patients.
The limitations of conventional treatments
One of the limitations of conventional treatments is that they primarily focus on wound healing. While this is essential in the management of venous leg ulcers, it does not address the underlying cause of the condition, which is chronic venous insufficiency and varicose veins . Therefore, even after the wound in venous leg ulcers has healed, the underlying chronic venous insufficiency remains, and the ulcer may reoccur.
Another limitation is the lack of personalised treatment options. Each patient’s condition is unique, and the severity of the venous leg ulcer and the underlying chronic venous insufficiency can vary. Therefore, a one-size-fits-all approach may not be effective in managing venous leg ulcers.
Innovative treatments for venous leg ulcers
Recent advancements in the field of chronic venous hypertension and leg ulcer treatment have led to innovative treatments that address the underlying cause of venous leg ulcers, chronic venous insufficiency and varicose veins. These treatments offer personalised options that are tailored to each patient’s condition, improving the chances of successful management.
Compression Therapy: A Game-Changer in Venous Leg Ulcer Treatment
Compression therapy has been around for many years and is a tried-and-tested method for managing venous ulcers. However, recent advancements have led to the development of more effective compression therapy options for chronic ulcers and leg ulcers. These include multilayer compression bandages, intermittent pneumatic compression, and adjustable compression devices.
Multilayer compression bandages consist of multiple layers of compression that are applied to the legs. This helps to reduce swelling and improve blood flow to the lower leg, promoting healing. Intermittent pneumatic compression bandaging involves the use of a device that inflates and deflates to improve blood flow and reduce swelling.
Adjustable compression devices, such as the Flexitouch system, allow for personalised compression therapy, which can be adjusted to each patient’s condition.
Advanced Wound Dressings for Venous Leg Ulcers
Advanced wound dressings have also seen significant advancements in recent years. These include the use of bioactive dressings, which contain growth factors that promote healing and reduce inflammation. Antimicrobial dressings, which contain agents that prevent infection, are also available. Additionally, smart dressings that change colour when an infection is present can alert healthcare professionals to the need for further treatment.
Bioengineered Skin Substitutes for Venous Leg Ulcers
Bioengineered skin substitutes are an exciting development in the field of venous ulcer treatment. These substitutes are made from living cells and can be used to replace damaged skin. They promote healing and reduce the ulcer healing risk of infection, leading to faster healing times. They are also personalised to each patient’s condition, offering an effective treatment option.
Bioengineered skin substitutes are typically composed of living cells, extracellular matrices, and biomaterials that mimic the structure and function of natural skin. These substitutes can be applied directly to the wound bed, providing a supportive environment for cell proliferation, angiogenesis, and re-epithelialization.
One type of bioengineered skin substitute commonly used for venous ulcers is the acellular dermal matrix (ADM). ADM is a scaffold made from human or animal-derived collagen that has been processed to remove cellular components. When applied to the wound, ADM provides a framework for the infiltration of host cells dead tissue, and the regeneration of new tissue.
Another type of bioengineered skin substitute is the living cell-based skin substitute. These substitutes are composed of living cells, such as keratinocytes and fibroblasts, embedded within a matrix. When applied to the wound, the living cells promote the formation of new tissue and accelerate wound healing.
Clinical studies have shown promising results with the use of bioengineered skin substitutes in the treatment of venous ulcers. In a multicenter randomised controlled trial, patients who received bioengineered skin substitutes experienced faster healing rates and a higher proportion of complete wound closure compared to those treated with conventional dressings.
The development of bioengineered skin substitutes has opened up new possibilities for the treatment of venous ulcers. These innovative therapies have the potential to improve outcomes for patients with chronic wounds where venous ulcers form and offer a viable solution for those who have failed to respond to conventional treatments.
PRP therapy for Venous Leg Ulcer
Platelet-Rich Plasma (PRP) therapy is a cutting-edge treatment that has shown promise in accelerating wound healing and improving outcomes for venous leg ulcers. PRP therapy involves extracting and concentrating platelets from a patient’s own blood, rich in growth factors and cytokines. These platelets stimulate cell regeneration, reduce inflammation, enhance blood supply, and fight infection. The process involves blood collection, centrifugation, activation, and application. Benefits of PRP therapy include faster wound closure, reduced recurrence, minimal invasiveness, and personalised treatment.
Emerging Technologies in Venous Leg Ulcer Treatment
Emerging technologies such as stem cell therapy and gene therapy offer promising treatment options for venous ulcers. Stem cell therapy involves the use of stem cells to repair damaged tissues, promoting healing. Gene therapy involves the use of genes to modify cells, leading to improved blood flow and reduced inflammation chronic venous leg ulceration.
While these treatments are still in the early stages of development, they offer hope for the future of venous leg ulcer treatment.
Minimally Invasive Treatments for Chronic Venous Leg Ulcers
Chronic venous leg ulcers can be both physically and emotionally taxing for those affected. However, modern medicine offers a range of minimally invasive treatments that have revolutionised the management of these debilitating wounds.
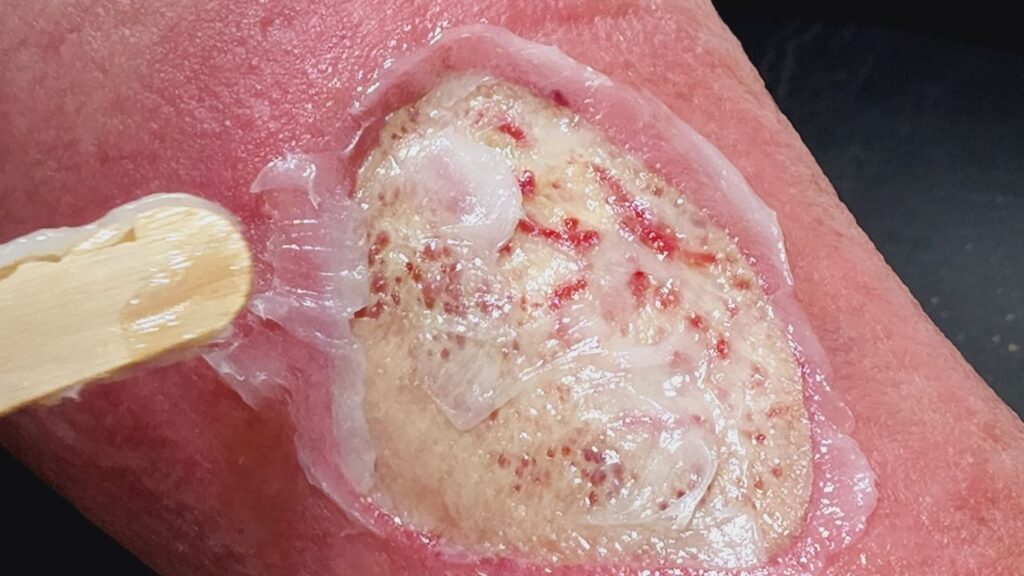
Endovenous Laser Ablation (EVLA)
EVLA is a cutting-edge procedure that targets the underlying cause of chronic venous leg ulcers: venous insufficiency. Using laser energy, this treatment closes off faulty veins, redirecting blood flow to healthier vessels. By addressing the root of the problem, EVLA has shown remarkable success in promoting wound healing and preventing venous ulcer recurrence throughout.
Radiofrequency Ablation (RF)
Similar to EVLA, RF is a minimally invasive technique designed to treat venous insufficiency. Instead of laser energy, RF employs radiofrequency waves to seal off problematic veins. This procedure has proven highly effective, providing relief to many suffering from chronic venous leg ulcers. Its minimal discomfort and quick recovery time make it a preferred choice for many patients.
Sclerotherapy
Sclerotherapy is a versatile treatment that can be used to address various types of problematic veins, including those associated with chronic venous leg ulcers. A specialised solution is injected into the affected vein, causing it to collapse and eventually be absorbed by the body. Sclerotherapy is particularly useful for smaller veins and can be a valuable adjunct to other treatments.
The Benefits of Minimally Invasive Treatments
These procedures offer numerous advantages for patients dealing with chronic venous leg ulcers:
– Minimized Discomfort:
Compared to traditional surgical interventions, minimally invasive treatments typically involve less pain and shorter recovery times.
– Outpatient Procedures:
Many of these treatments can be performed in an outpatient setting, allowing patients to return home on the same day.
– Preservation of Healthy Tissue:
Minimally invasive techniques focus on treating the underlying venous insufficiency while preserving surrounding healthy tissue.
– High Success Rates:
Studies have shown that these treatments are highly effective in promoting wound healing and reducing the recurrence of chronic venous leg ulcers.
Skin Grafts for Venous Ulcers
Skin grafting is a surgical procedure that involves transplanting healthy skin tissue from one area of the body to cover a wound or area of skin loss. It is particularly beneficial for venous ulcers that have failed to respond to other treatment modalities.
There are several types of skin grafts, including Full-Thickness Skin Grafts (FTSG), Split-Thickness Skin Grafts (STSG), and Meshed Grafts. The grafting procedure involves preparing the recipient site, harvesting the graft, and suturing the harvested skin onto the recipient site. Adequate post-operative care is essential for successful graft integration.
Skin grafts offer several advantages for treating venous ulcers, including promoting wound closure, reducing pain and discomfort, and preventing infection. However, factors such as overall health, vascular status, and the availability of a suitable donor site must be considered.
Conclusion: The future of venous ulcer treatment
In addition to compression therapy, advanced wound dressings, and bioengineered skin substitutes, emerging technologies are shaping the future of venous ulcer treatment. These technologies aim to enhance the effectiveness of existing treatments and introduce new therapeutic modalities to improve patient outcomes.
One such emerging technology is the use of negative pressure wound therapy (NPWT) in the management of venous ulcers. NPWT involves the application of a vacuum system to the wound bed, promoting wound healing through the removal of excess exudate, reduction of edema, and stimulation of tissue perfusion. This therapy has been shown to accelerate wound healing, reduce wound size, and improve the quality of granulation tissue in venous ulcers.
Another promising technology is the use of low-level laser therapy (LLLT) for the treatment of venous ulcers. LLLT involves the application of low-power lasers or light-emitting diodes to the wound area, stimulating cellular processes and promoting tissue regeneration. Studies have demonstrated the beneficial effects of LLLT in reducing pain, promoting wound healing, and improving the overall quality of life for patients with venous ulcers.
Additionally, advancements in telemedicine and digital health solutions are revolutionising the way chronic venous ulcers are managed. Remote monitoring systems, smartphone apps, and wearable devices allow healthcare professionals to track patients’ progress, provide real-time feedback, and offer personalised treatment plans. These technologies enable early intervention, improve patient compliance, and enhance the continuity of care for individuals with venous ulcers.
In conclusion, emerging technologies have the potential to transform the field of venous ulcer treatment. From negative pressure wound therapy and low-level laser therapy to telemedicine and digital health solutions, these innovations offer new avenues for improving patient outcomes and advancing the management of venous ulcers.