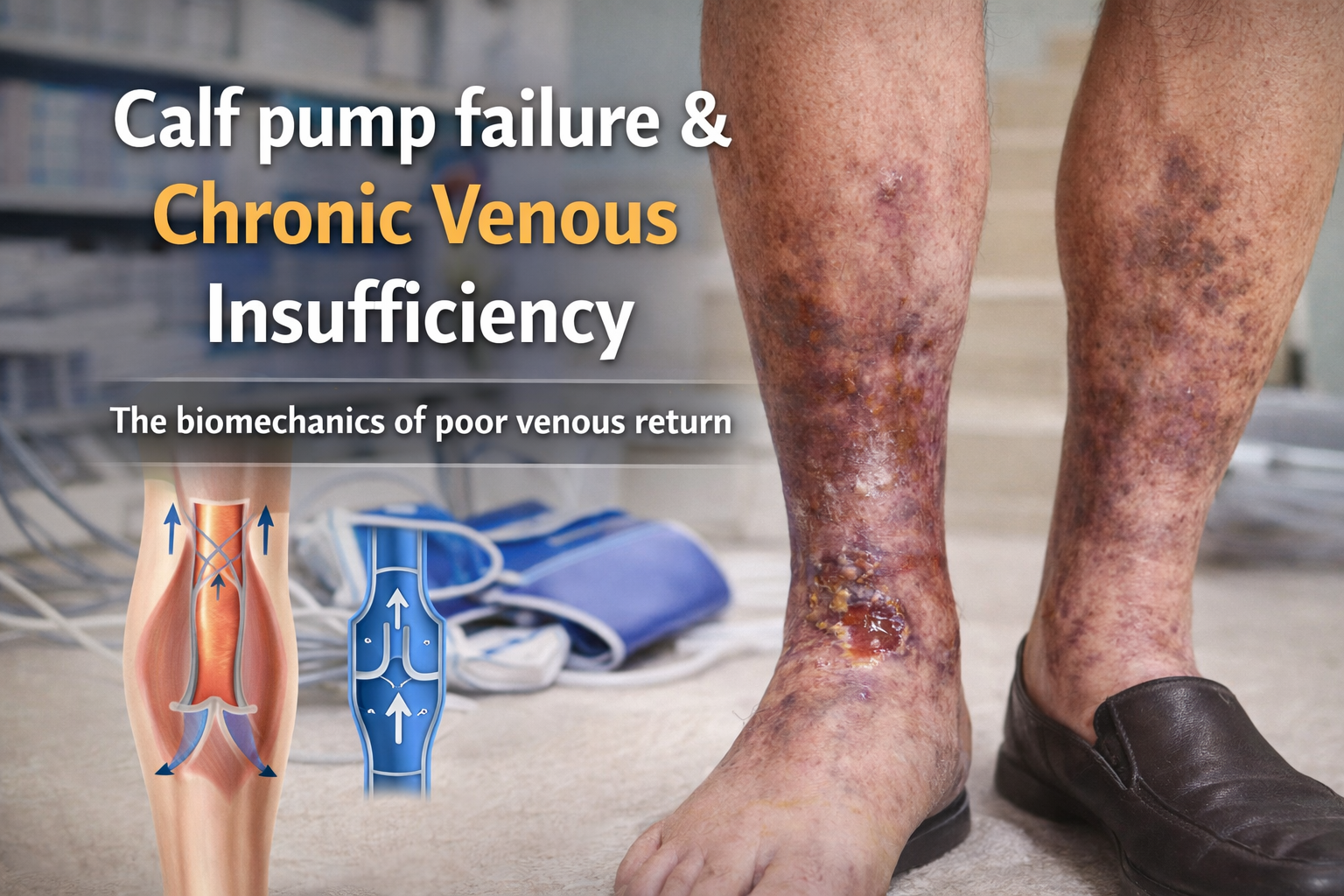
The calf pump: the hidden engine of venous return
The calf muscle pump is the primary biomechanical driver of venous return from the lower limb. During walking, ankle flexion and contraction of the soleus and gastrocnemius muscles compress deep veins, propelling blood proximally toward the heart. Venous valves maintain unidirectional flow and prevent reflux between contraction cycles.
Under normal conditions, this system:
empties deep venous reservoirs during ambulation
reduces ambulatory venous pressure
prevents distal venous pooling
protects microcirculation from sustained hydrostatic load
Because upright humans operate against gravity for most of the day, the calf pump is not optional. It is essential infrastructure for venous health. When it fails, the consequences accumulate slowly but predictably.
Chronic venous insufficiency (CVI) is rarely a sudden disease. It is usually the downstream effect of progressive calf pump dysfunction.
What calf pump assessment is actually measuring
Calf pump assessment evaluates whether the lower limb can effectively evacuate venous blood during movement.
Clinically, this is not a single measurement. It is a composite functional evaluation involving:
1. Ankle mobility
Restricted dorsiflexion reduces calf compression efficiency. Even small losses in ankle excursion significantly reduce venous emptying volume per step.
Common contributors include:
sedentary behaviour
prior ankle injury
osteoarthritis
immobilisation history
prolonged boot use in occupational settings
2. Muscle contraction strength
The soleus acts as the primary venous pump during walking. Weakness reduces pressure transmission into deep veins.
Loss of strength may result from:
ageing
inactivity
neuropathy
spinal pathology
post-operative deconditioning
3. Venous valve competence
Even a strong pump becomes ineffective if valves fail to maintain directional flow. Reflux converts propulsion into oscillation rather than transport.
4. Ambulatory venous pressure reduction
The defining physiological test of calf pump performance is how effectively walking lowers venous pressure at the ankle. In normal limbs, pressure drops rapidly with movement. In dysfunctional systems, pressure remains elevated.
Why the calf pump fails
Calf pump failure is rarely caused by a single defect. It usually reflects interacting impairments across movement, muscle, valves, and venous structure.
Reduced ankle range of motion
Loss of dorsiflexion limits venous compression amplitude. This reduces ejection fraction from deep veins with each step. Over thousands of daily steps, the cumulative deficit becomes physiologically significant.
Muscle inactivity
The soleus is designed for endurance activation throughout standing and walking. Modern sedentary behaviour removes this stimulus.
Without repeated contraction:
venous capacitance increases
emptying efficiency declines
reflux tolerance worsens
Over time, the system adapts to underuse.
Valve incompetence
Valve failure transforms the venous column from a segmented pressure system into a continuous hydrostatic column extending from the heart to the ankle.
The result is persistent distal venous hypertension during standing.
Deep venous obstruction
Previous thrombosis alters flow geometry and increases resistance within the system. Even partial obstruction increases reliance on collateral pathways that are less efficient under load.
The calf pump must then work harder to achieve the same effect.
Often, it cannot.
How pump failure becomes chronic venous insufficiency
CVI develops when ambulatory venous pressure remains elevated for prolonged periods across months or years.
This sustained pressure produces predictable downstream changes.
Stage 1: venous hypertension
Persistent distal pressure increases capillary filtration into surrounding tissue. Interstitial fluid accumulation becomes visible as dependent oedema.
Initially reversible.
Eventually persistent.
Stage 2: inflammatory signalling
Chronic venous hypertension activates endothelial cells and leukocytes. Microvascular permeability increases. Plasma proteins leak into surrounding tissue.
This initiates long-term dermal change.
Stage 3: skin and subcutaneous fibrosis
Extravasated proteins stimulate fibroblast activation. Over time:
lipodermatosclerosis develops
skin thickens
pigmentation appears
elasticity declines
The gaiter region becomes structurally altered.
Stage 4: ulceration
When microcirculatory oxygen exchange becomes impaired, tissue tolerance falls below normal mechanical stress thresholds.
Minor trauma becomes non-healing injury.
Venous ulceration represents end-stage pump failure physiology rather than a local skin disorder.
What clinicians look for during calf pump assessment
Effective assessment integrates observation, movement testing, and haemodynamic evaluation.
Typical indicators of dysfunction include:
reduced ankle dorsiflexion during gait
absent heel rise during walking
inability to perform repeated single-leg heel raises
persistent lower-leg oedema
gaiter-zone pigmentation
varicosities with reflux
delayed venous refill time
reduced ejection fraction on plethysmography
No single marker confirms failure.
Instead, the pattern reveals the diagnosis.
Why calf pump failure is often missed early
The calf pump deteriorates gradually. Early dysfunction rarely produces symptoms strong enough to prompt investigation.
Patients often report:
heaviness late in the day
ankle swelling after work
tightness in footwear
reduced walking endurance
These are frequently attributed to fatigue rather than venous mechanics.
By the time visible skin change appears, the system has usually been failing for years.
CVI is therefore less a sudden condition than the visible endpoint of long-term haemodynamic inefficiency.